Spider veins can be treated with lasers & sclerotherapy. Facial spider veins do best with vascular lasers, whilst leg veins respond optimally to sclerotherapy injections. Treatments are comfortable & typically take between 15 to 30 minutes to perform. Medicare rebates apply to most cases of facial veins. There are no rebates for small diameter spider leg veins.
Key Points
- Spider veins on the lower extremities are best treated with sclerotherapy
- Veins on the face are best treated with vascular lasers
- Sclerotherapy involves injection of a ‘sclerosant’
- A sclerosant causes irritation to the vessel wall, resulting in closure
- It takes between 1-3 sclerotherapy sessions to obtain the best results
Spider Vein Treatment at a glance
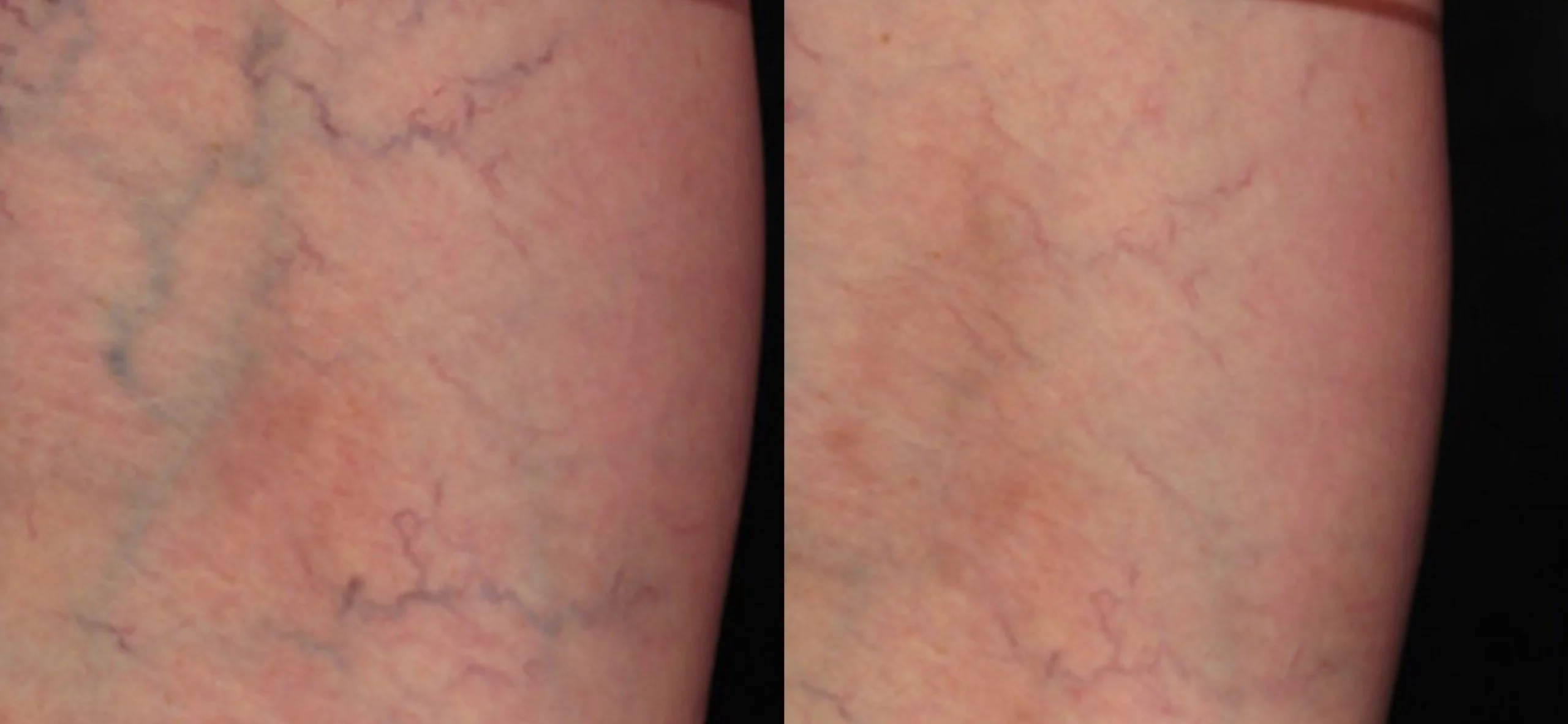
Our results speak for themselves
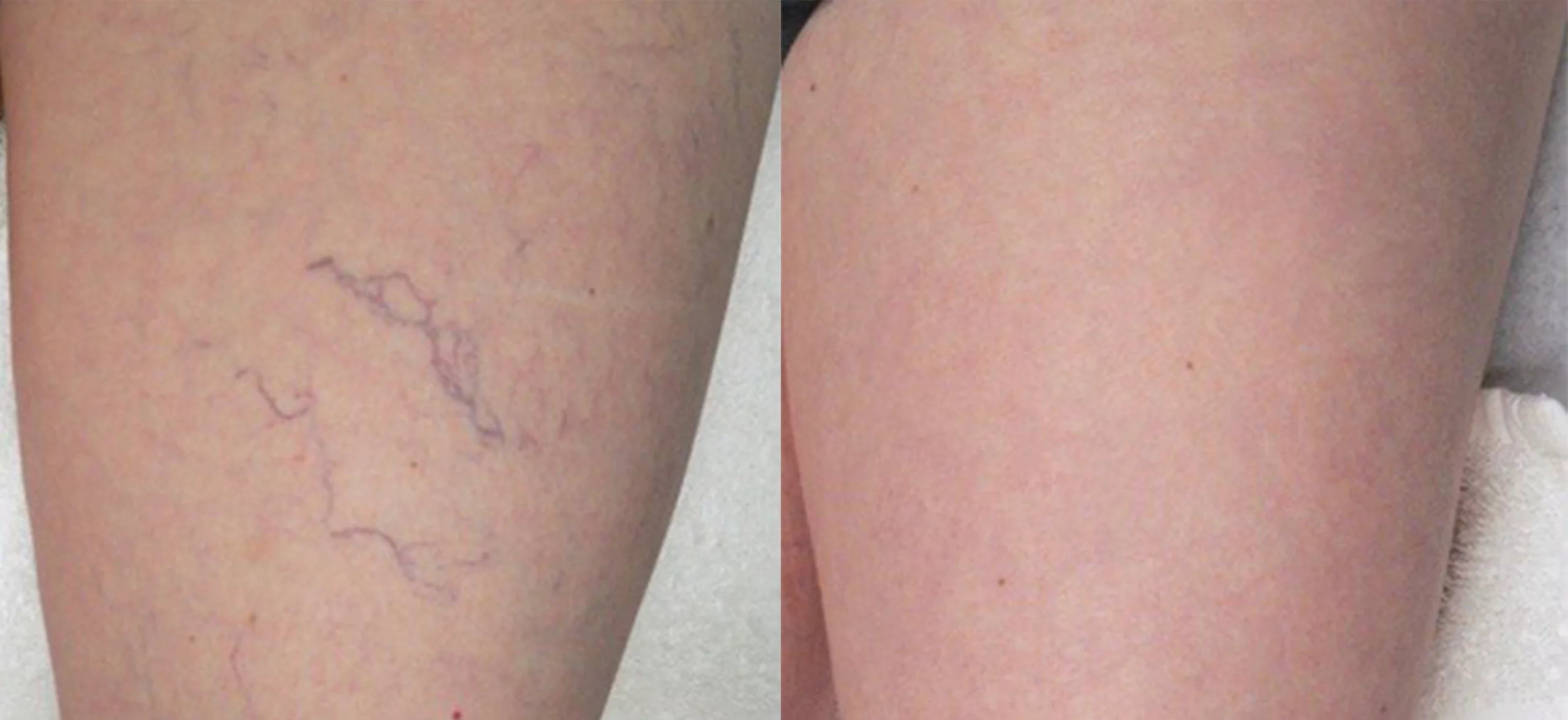
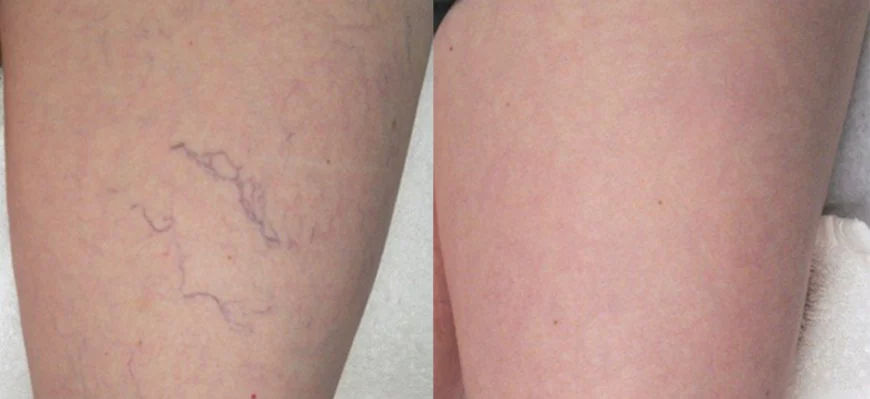
Sclerotherapy is an effective method for treating spider veins on the legs. 1- 3 sessions for optimal outcomes.
Ask us more about this treatmant
Preferred Consultation
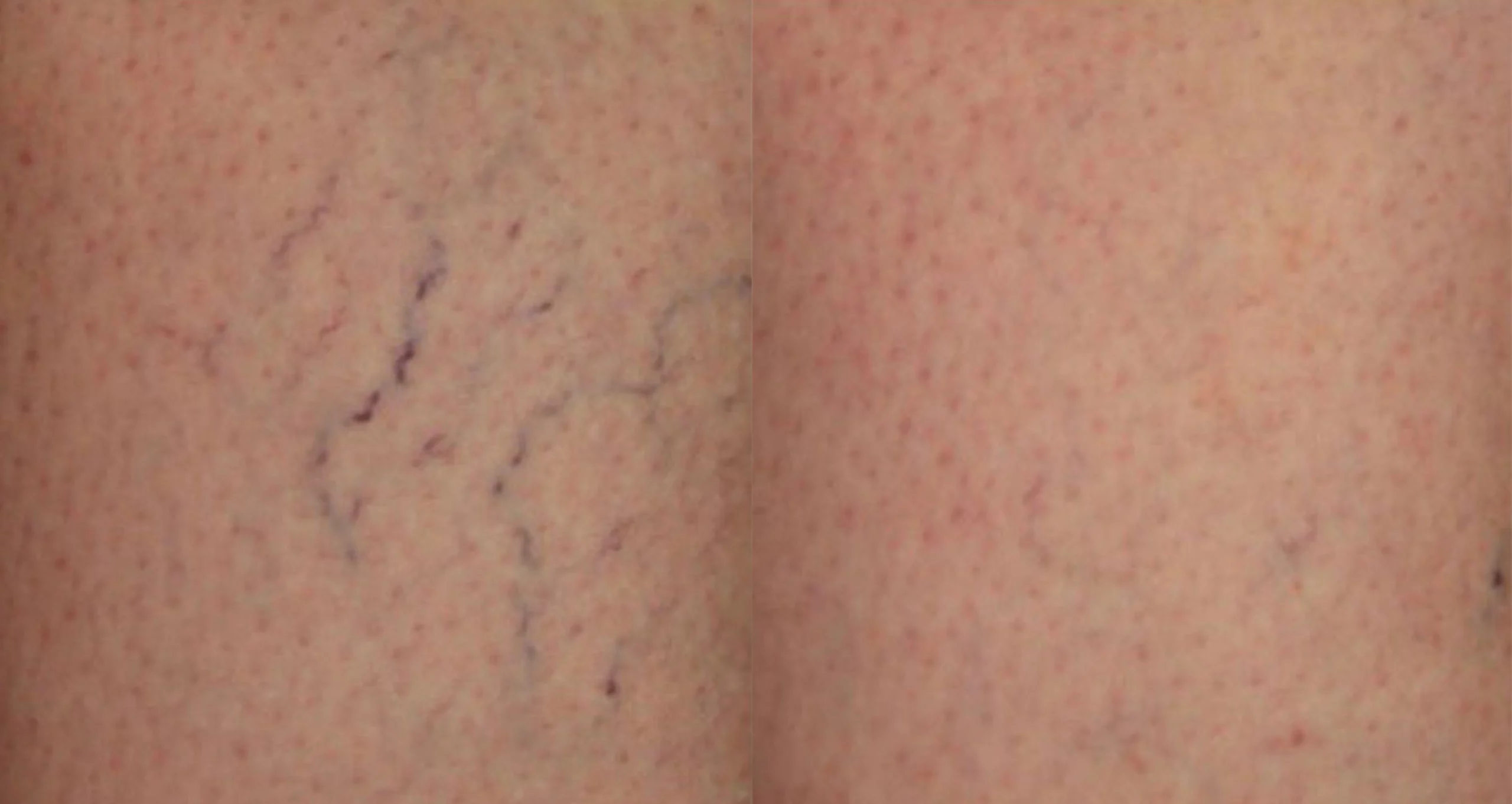
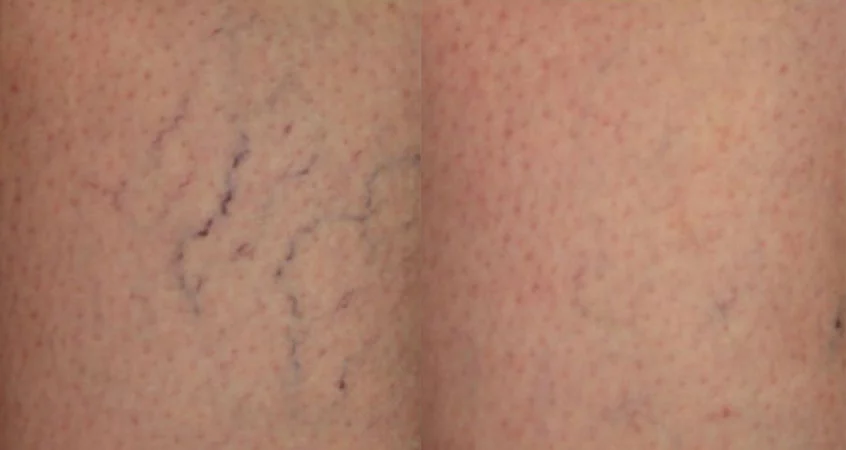
Sclerotherapy more effective than lasers for treating spider veins on the legs. 1- 3 sessions.
Ask us more about this treatmant
Preferred Consultation
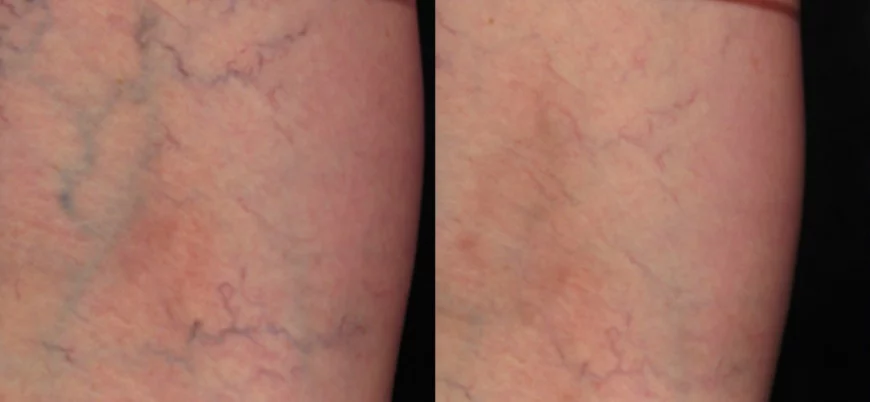
Sclerotherapy more effective than lasers for treating spider veins on the legs. 1- 3 sessions.
Ask us more about this treatmant
Preferred Consultation
FAQs
How do we treat leg veins?
The treatment of choice is with sclerotherapy. This involves manual injection of a chemical into the lumen of the spider vein, destroying the lining of the blood vessel.
This does not harm the circulation – it improves it by eliminating the abnormal, unnecessary vessel. Sclerotherapy works much better than lasers for lower limb spider veins.
How do we treat facial veins?
Facial veins are treated with vascular lasers. We employ state of the art lasers including the very latest VBeam Prima & Derma V lasers.
Superficial veins are treated with 532 nm or 595 nm lasers.
Deep veins are treated with 1064 nm lasers.
Learn more (link to vascular lasers in the vascular laser section)
Do spider veins on the legs respond to laser vein removal?
They can, however simple sclerotherapy is often better. Though we have the most advanced laser systems, we find that sclerotherapy provides better, more consistent & longer lasting results compared to laser.
The exception to this rule is with larger diameter veins. These vessels respond well to endovenous laser ablation conducted by a vascular surgeon in an operating room.
What is the difference between spider veins & varicose veins?
Varicose veins are larger. Think of them as major rivers, whilst spider veins are small creeks. Varicosities are green in colour & often protrude from the skin. They are often symptomatic & may be associated with pain when standing for long periods.
Spider veins are red-pink to purple in colour & measure between 0.5 to 2.5 mm in diameter. They don’t (usually) cause symptoms but may appear unsightly.
At Cutis Dermatology Brisbane, we only treat spider veins. Deeper feeding varicose veins require treatment by a vascular surgeon. If you have larger varicose veins associated with spider veins, you should ideally have these treated before spider vein treatment. The rule of thumb is to treat the ‘rivers’ before the ‘creeks’, namely big to small.
For varicosities, ask your GP to refer you to Dr Andrew Cartmill, vascular surgeon in Brisbane.
When is ultrasound useful?
Ultrasound guidance is useful for the management of larger varicose veins. This imaging procedure is employed to visualise the vessels during injection as it helps the clinician visualise where the solution is going during the procedure.
For treatment of superficial spider veins, most patients do not require ultrasound, unless we suspect a deeper ‘feeding’ vessel.
How many sessions will it take to remove spider veins on the legs?
The number of treatment sessions depends on the size, depth, area & extent of vessels. For thread veins & small spider veins, only one session is required. For more extensive veins, you may require up to 3-5 sessions for optimal outcomes.
Treatments are spaced 6-8 weeks apart to minimise irritation of previously treated sites.
When will I see results?
Depending on the sclerosant we employ, results can be immediate or delayed for several weeks.
Will spider veins recur following sclerotherapy?
If you are prone to spider veins, chances are you will get more. For most, you should get remission of 3- 6 years. Treatments cannot prevent you from getting more spider veins in time. Higher recurrence is seen in-
- Patients who have larger feeding vessels & varicose veins (hence treat big to small)
- Those with radiating mat like vessels
- A family history of varicose veins
- Patients who stand up for long periods of time
- Those who have a higher BMI
- Patients who don’t complete their post-operative compression stocking application times
Is spider vein treatment painful?
Treatments are well tolerated. For leg veins there may be some mild stinging during the procedure itself. For laser spider vein removal, we use lasers with cryogen spray, making the procedure extremely comfortable.
Does Medicare cover spider vein treatments & what are the costs?
Medicare partially covers spider vein laser removal on the face, however there is no rebate for small spider veins on the lower limbs. As a guide:
Spider vein removal on the lower limbs/legs: $440 per 20 minutes session. $795 for a 40-minute session.
Spider vein removal on the face: $260 – $550 out of pocket (depending on the consultant)
Sclerotherapy – small area ($200-$250)
Sclerotherapy – medium/large area ($350-$400)
*If you are after budget treatments, please make an appointment with our dermatology nurses. Their fees are typically half that of our senior dermatologists. For large varicose veins that are symptomatic, a Medicare rebate may apply.
What is our experience with treating spider veins?
Our senior nurses have over 25 years of experience (that’s not a typo) of experience in sclerotherapy, having treated thousands of patients in that time.
Our dermatologists have two decades of laser experience in the management of facial veins & redness.
How do I get started?
A real time appointment will allow us to assess the extent of your veins, in addition to performing a clinical examination. Book a free consultation with our nurses.
*T+C applies. Consult fee deducted from procedural fee.
**Consultant dermatologist fee applies.
What are the possible side effects of leg spider vein treatment?
Though we are skilful with sclerotherapy, there are associated adverse outcomes. Most will settle down with time & include:
- Discolouration & post inflammatory hyperpigmentation is not uncommon. This occurs in up to 25% of cases & occurs along the course of the vein. It resolves within 8 months, pico lasers can speed up resolution.
- Pain & muscle spasm: are rare side effects. They can occur if your vessel walls are super thin. Settles within 15 to 30 minutes.
- Telangiectatic matting: or new vessel formation can develop in 5-10% of cases. These will persist for 4-8 months; the vast majority will resolve with time.
- Ulceration: less than 0.1% of cases. This is due to extravasation of sclerosant into the surrounding tissues. This is usually seen around the ankles in mature patients. Scaring may result. If you experience ulceration, ensure that we promptly review your case.
- Injection site swelling may be prolonged in some. The use of compression stockings will reduce this.
- Superficial vein irritation occurs in 0.1% of cases. Best treated with compression stockings & anti-inflammatory medications.
- Allergies to sclerosants other than hypertonic saline are rare, but reported.
How can side effects be reduced?
On our part we ensure that we carefully inject the sclerosant of choice into the vessel wall, that’s given.
From your part, the use of compression stockings will markedly reduce the risk of unwanted side effects. Our nurses will guide you as to the application frequency & duration.
What is the recovery like following spider vein sclerotherapy?
Your clinician will provide you with a list of dos & don’ts. It goes something like this-
- Wear your compression stockings as directed
- Avoid super strenuous activity for 72 hours post procedure.
- Normal paced walks are encouraged, 30 minutes daily.
- Avoid hot baths for 10 days.
- Avoid standing for long periods- move!
How does sclerotherapy work?
Sclerotherapy entails the use of a sclerosant, typically a chemical or hypertonic saline. These agents irritate the vessel wall, resulting in collapse of the spider vein without damage to the surrounding tissue. Hence it is vitally important to inject the chemical directly into the lumen of vessels.




