Atopic dermatitis is the most common form of eczema, a condition that causes the skin to become itchy, dry & can cause rashes, scaly patches, blisters, & skin infections. It is most frequently found in children but tends to resolve when they get older. The specialist dermatologists at our Brisbane clinics can guide you as to how to effectively manage atopic dermatitis.
Treatments we offer at Cutis Dermatology include:
- Sensitive skin care
- Allergy Testing
- Narrowband Phototherapy
- Children’s Dermatology
Our results speak for themselves
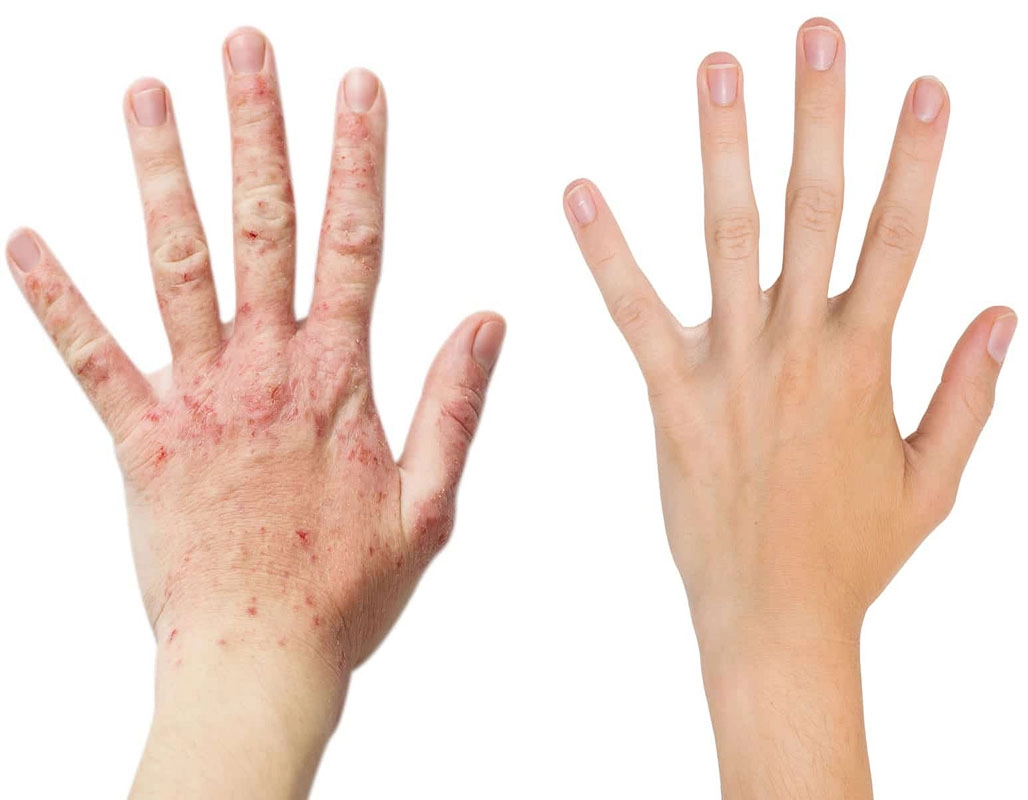
Before
After
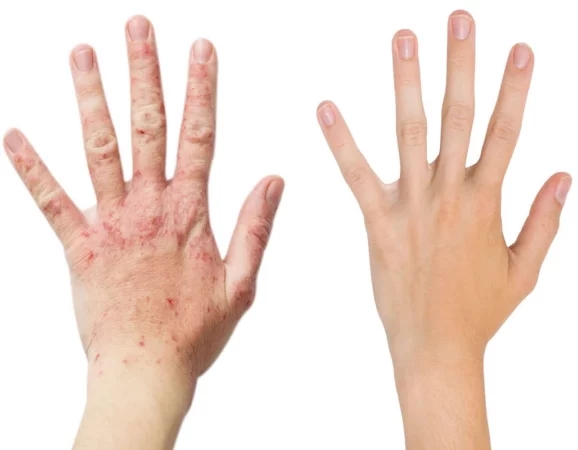
Emollients, anti-inflammatory medications
& soap substitutes are the mainstay for
eczema management
Ask us more about this treatmant
Preferred Consultation
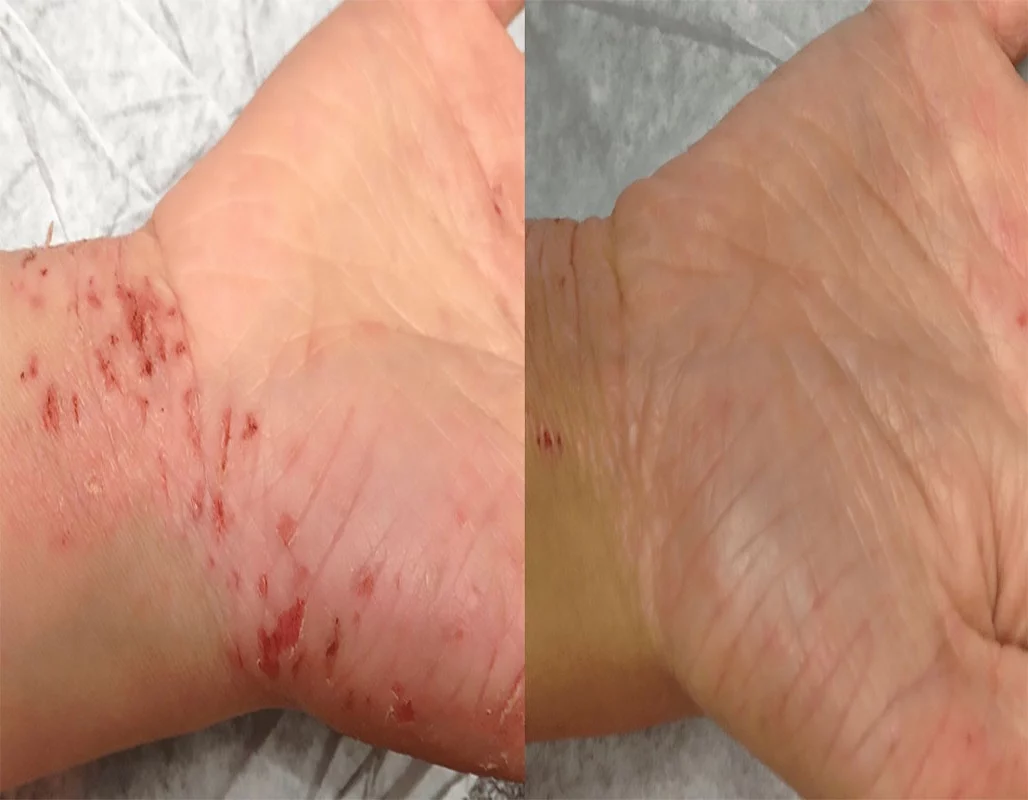
Before
After
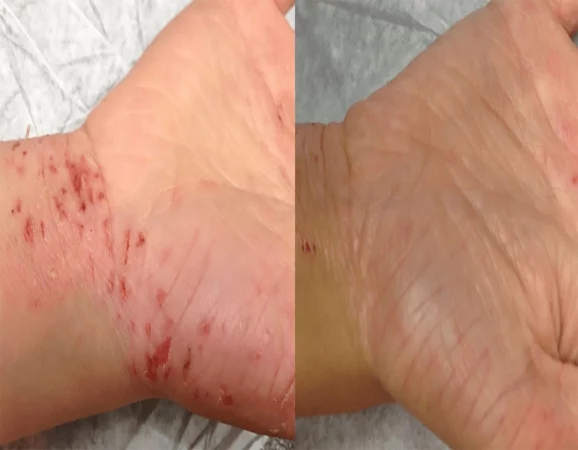
Emollients, anti-inflammatory medications
& soap substitutes are the mainstay for
eczema management
Ask us more about this treatmant
Preferred Consultation
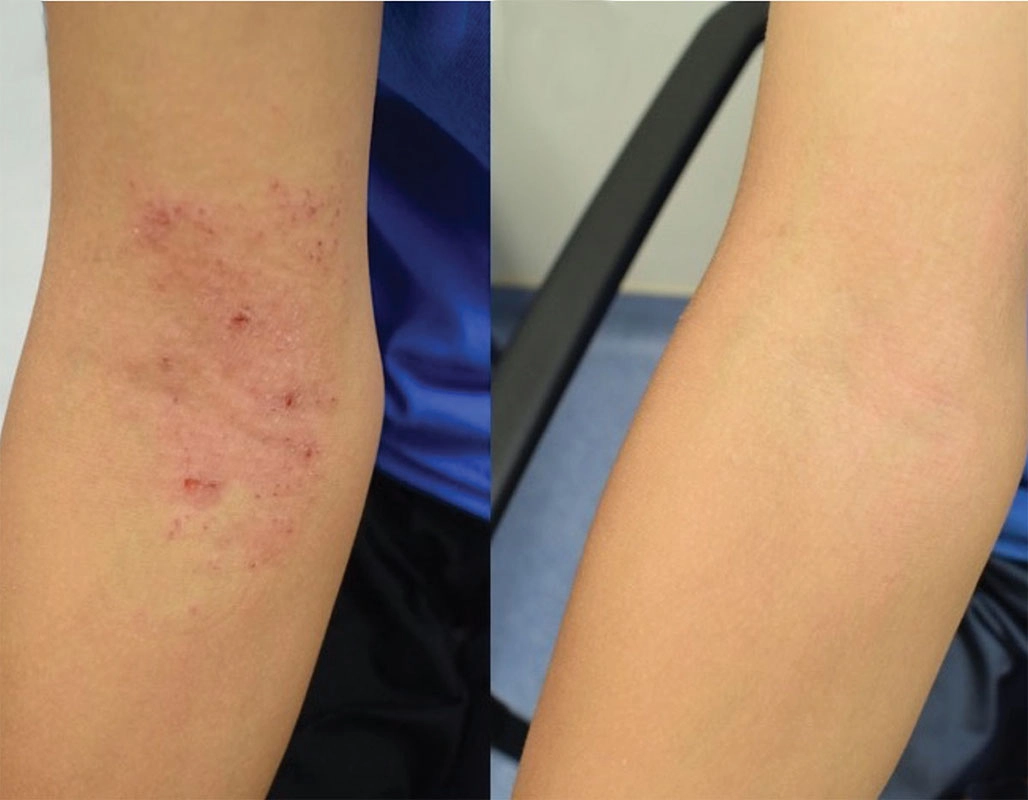
Before
After
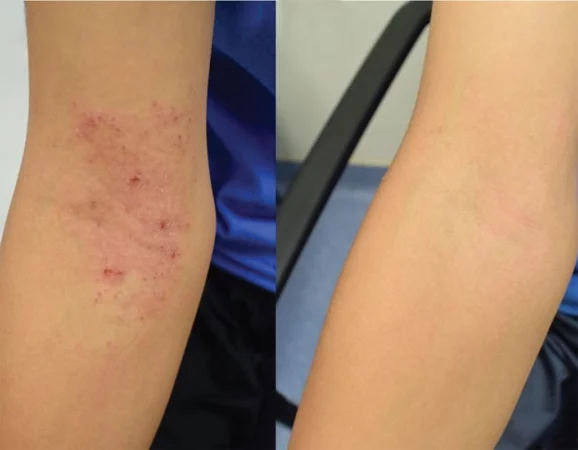
Narrowband phototherapy can reduce the
requirement for steroids when treating
eczema
Ask us more about this treatmant
Preferred Consultation
Treatments for Eczema
Our specialist dermatologists are experienced in the management of atopic dermatitis in all ages- from neonates to adults. We provide non-drug treatments such as narrowband phototherapy.
FAQs
What is atopic eczema?
Atopic eczema is a very common inflammatory skin condition. It is also known as atopic dermatitis. The word atopic refers to immune conditions, and ‘Eczema’ is a term that comes from the Greek word ‘to boil’ which is related to symptoms like red, dry, itchy skin.
There are different types of eczema, but atopic eczema (dermatitis) is the most famous one. The most associated symptoms are rash, itchiness, dry & cracked skin, which may lead to blisters & skin infections.
Atopic eczema is more common in children, but it can also happen to adults. It is a long-term chronic condition that could erupt from childhood, however, there are cases where it is completely resolved as they get older.
What causes atopic eczema?
Dermatologists consider atopic eczema to be an immune problem, mainly caused by increased inflammation. Environmental & genetic factors play the major role. Although there is no exact cause to it, many contributing factors can cause atopic eczema to flare up.
Alteration in the skin barrier or inherited genes can cause an irritant or an allergen from outside or inside the body to alert the immune system to produce inflammation, or a flare-up, on the surface of the skin. This inflammation causes symptoms like red itchy skin or lead to developing a rash or infection.
If you have a family history of atopic eczema, you’re more likely to have it too, but atopic eczema is not a contagious condition. Emotional stress and hormones may also contribute to it, but there is no clear reason why.
What are common eczema flare factors?
Also, there are different environmental causes that could initiate inflammation, including:
- Irritants like soaps, detergents, fragrances, shampoos, & disinfectants.
- Food like milk and soy products
- Hot and cold temperatures may bring out eczema. Perspiration also can be a cause.
- Allergens as in Dust mites, pets, pollens, & mould
What are the symptoms of atopic eczema?
The main symptom of atopic eczema is the rash, it can be found anywhere in the skin, but it often forms in the creases of your elbows, knees, wrists, & /or neck. The rash may appear as coin-sized areas of inflammation and have small bumps which could leak fluid or cause infection if you scratch them.
Frequent scratches can cause rough, leathery, or scaly skin, appearing as scaly patches. Skin in areas where the rash appears may turn lighter or darker or get thicker. Infants usually get a rash on their scalp and cheeks.
The rashes are typically red, itches, dry cracked, and sore. You may also see water retaining blisters in the severe phase of atopic eczema.
How do dermatologists diagnose atopic eczema?
Dermatologists diagnose atopic eczema by examining your skin & reviewing your family history. Blood lab tests are rarely used in the diagnosis of eczema.
Patch testing is also used to rule out other suspected conditions or confirm accompanying conditions to eczema. Your doctor may also suspect food allergies.
Dermatologists often take swaps of the infected skin to check for viral or bacterial infections that may be caused by eczema.
How is atopic eczema treated?
There is no definite cure found for eczema, but it is manageable and can be resolved over time. It tends to clear out in most children after reaching adulthood, although they still need to avoid any irritants or skin dryness.
The treatment approach for dermatologists is using topical creams in eczema. Oral medications can be taken in severe conditions.
What are emollients & why are they first line therapy for patients?
This therapy depends on constant moisturizing of your skin, whether frequently applying moisturizers or washing with a moisturizer instead of soap. This will help decrease any flare-ups & make your eczema more manageable.
Moisturizers or “emollients” when applied frequently, will help your outer layer of skin and protect it from any damage or infections. Drier skin will need a more concentrated moisturizer and more frequent application.
Aqueous creams may irritate the skin more, however, a greasy moisturizer is better but pick one you are comfortable with. Also, if eczema is frequently associated with infections, your dermatologist may recommend antiseptic moisturizers.
How do steroids treat eczema, & are they safe?
Topical steroids are used in eczema for redness & itching. Your dermatologist will choose the best type of steroids according to your case.
Topical steroids are safe under supervision, your specialist will take great care to monitor for side effects including skin thinning.
How do antibiotics & antiseptics treat eczema?
Antibiotics are used in the treatment of infections caused by eczema. Infections can make your skin become wet and crusted, which causes more damage to your skin.
Antiseptics are preferred to be used in a combination with moisturizers, as they tend to be very drying alone. A simple formulation consists of bleach added to baths. Commercial preparations contain triclosan.
What is phototherapy & why is it great for atopic dermatitis?
Natural light can improve eczema; however, UV has cancer causing wavelengths. Medical phototherapy filters out the dangerous wavelengths but efficiently delivers UV in a safe but highly effective treatment called narrowband phototherapy.
This treatment takes less than three minutes to perform & is covered under Medicare.
Learn more (link to phototherapy)
How long does it take for phototherapy to start working?
Narrowband phototherapy starts to work within a few sessions. In most cases the treatment goes something like this-
- Step one; control. This means combined treatments with phototherapy, prescription medications & emollients.
- Step two; taper. Your dermatologist will taper off the topical prescription creams.
- Step three; maintain. We then maintain your skin with phototherapy & simple moisturizer.
What is the safety data of phototherapy for atopic eczema?
This treatment has a very long safety record spanning over 3 decades. Phototherapy can be used in children, providing adequate eye protection is used.
This drug free way of treating eczema is preferred by most patients & parents. It can be stopped & restarted based upon your control of dermatitis.
What are steroid sparing agents used to treat eczema?
If your condition is not responding to topical steroids, calcineurin inhibitors are used to decrease any redness or inflammation. They are also used in case eczema is found in areas that are more susceptible to steroids side effects like the face, eyelid, armpits, and groin.
They may sting when you apply it, but it resolves over time. Furthermore, calcineurin inhibitors shouldn’t be applied if there is an infection, as calcineurin inhibitors may aggravate it. Be guided by your dermatologist.
What do antihistamines do?
Antihistamines are typically used at night to decrease any night scratches & help in getting rid of sleep disturbance. A favourite is Phenergan. It comes in tablet & liquid form.
What oral tablets can be used to treat eczema?
Oral drugs may be an option considered by your dermatologist in case of severe eczema, but they need special monitoring due to their risky side effects. Some options are:
- Oral steroids (prednisolone)
- Azathioprine
- Ciclosporin
- Methotrexate
- Mycophenolate mofetil
Can atopic eczema be caused by food allergy?
Specialists understand that food allergies & eczema are correlated in some patients. While not all atopic dermatitis patients have allergies, approximately 30 percent of children with moderate to severe atopic dermatitis will have an IgE-mediated food allergy.
Food allergies are not part of our usual investigation, as dermatologists are experts in controlling the skin side of things. We recommend evaluation by an immunologist or an allergy specialist with close supervision from a dietician.
What should I do if I think certain foods are causing my child’s eczema to get worse?
There are no definitive skin prick tests or blood tests that will tell us if certain foods may be the cause of eczema.
An allergist may suggest an elimination diet if foods are suggestive of flare ups. This involves elimination, stabilisation then a ‘re-challenge’. A rechallenge is required to confirm the suspicion.
A dietician will supervise an elimination diet as it is very important to replace the missing foods with other foods of similar nutritional value, this is especially important if cow’s milk is removed.
What are helpful tips to decrease eczema flare-ups?
There are some tips to deal with eczema flare-ups like:
- Avoid dry skin by moisturizing your skin daily (2 or 3 times a day) with a rich cream or ointment suitable for your skin type to protect you from any damage to your skin barrier
- If you are feeling itchy, apply cool compresses to the affected area or take a baking soda bath. These tricks will relieve the itchy feeling and help you avoid any scratching to your skin
- When you dry yourself after your bath or shower, don’t rub the towel on your skin, just dab lightly to avoid any friction or over-drying your skin
- Avoid fragrance products like detergents, cleansers, make-up, and choose fragrance-free options
- Wear loose cotton clothes or any loose soft fibres
- Avoid dealing with chemicals and wear gloves that are latex-free if you must
- Try to observe what causes your flare-ups to avoid it
- Take lukewarm baths
What are the complications of eczema?
Untreated atopic eczema could cause different complications including-
Chronic itchy, scaly skin: if you scratch your skin frequently or leave your skin dry for a long period of time, it can make it itchier, leading to a condition called neurodermatitis which is chronic itching and scratching. Eventually the skin will be discoloured, thick and leathery.
Skin infections: breakage of skin due to repeated scratching can open cracks for bacteria and viruses to enter in deeper skin layers and increase the risk of infections.
What’s the outlook for eczema?
Usually, atopic eczema resolves over time. It is slightly severe in childhood and resolves with getting older. However, some forms of eczema may be chronic throughout your life, but it can still be manageable.