Frontal fibrosing alopecia is a hair loss condition that is accompanied by scarring on the frontal scalp with frequent involvement of the eyebrows. Proposed triggers include hormonal changes, cosmetics & an abnormal autoimmune response. Our dermatologists at Cutis in Brisbane are experts in diagnosing & managing this condition.
Key points
- Frontal fibrosing alopecia is a scarring hair loss due to inflammation
- There is no clear cause of frontal fibrosing alopecia, but triggers including hormones and contact allergies have been postulated
- Redness, itchiness, and band-like hair loss pattern are the common symptoms of frontal fibrosing alopecia
- Management options include anti-inflammatory drugs, immune modulators as well as novel treatments including low level laser therapy
- Although there is no clear treatment, frontal fibrosing alopecia seems to slowly resolve after a few years. Spontaneous hair regrowth is very rare.
Frontal Fibrosing Alopecia at a glance
Our results speak for themselves
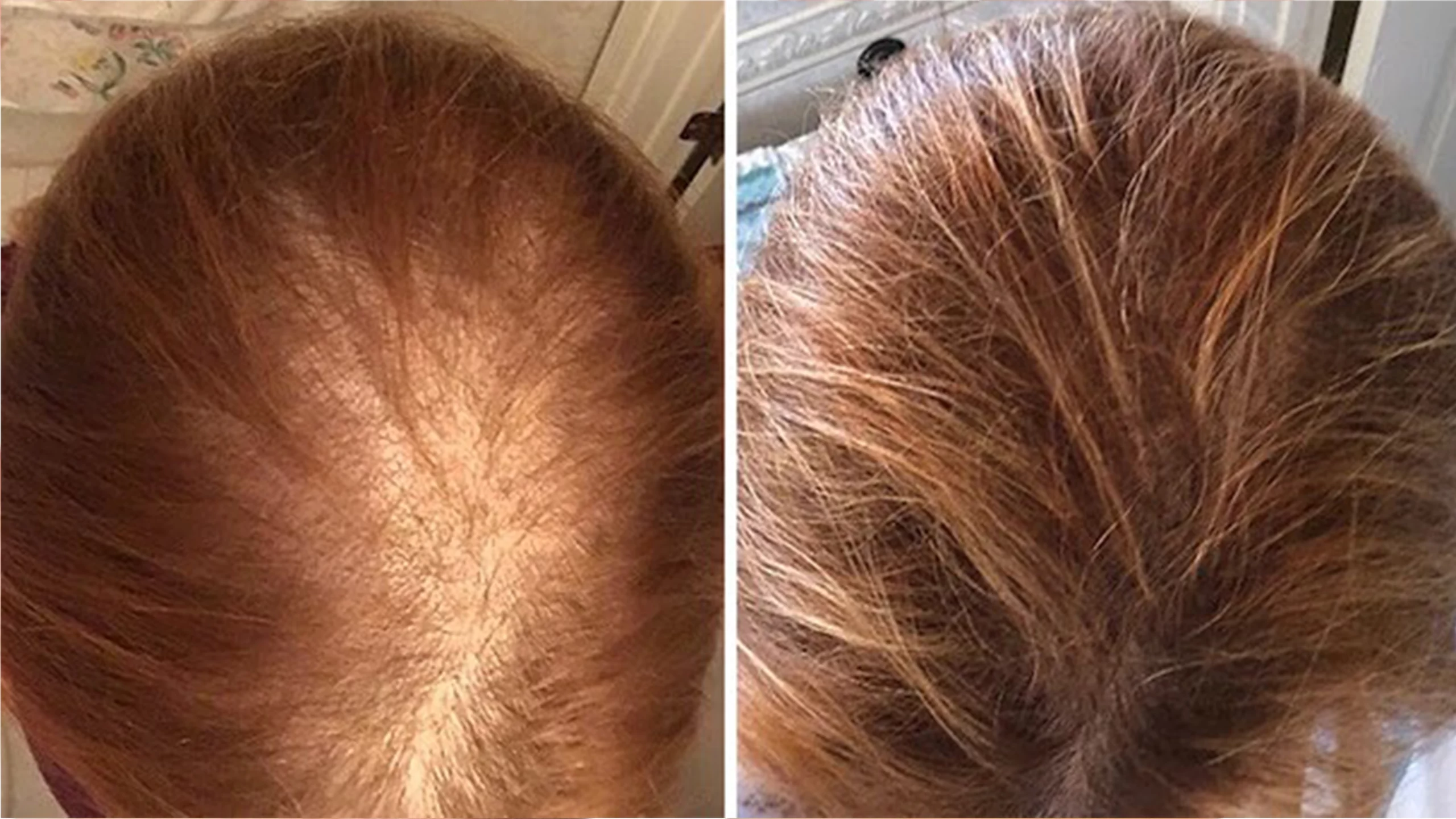
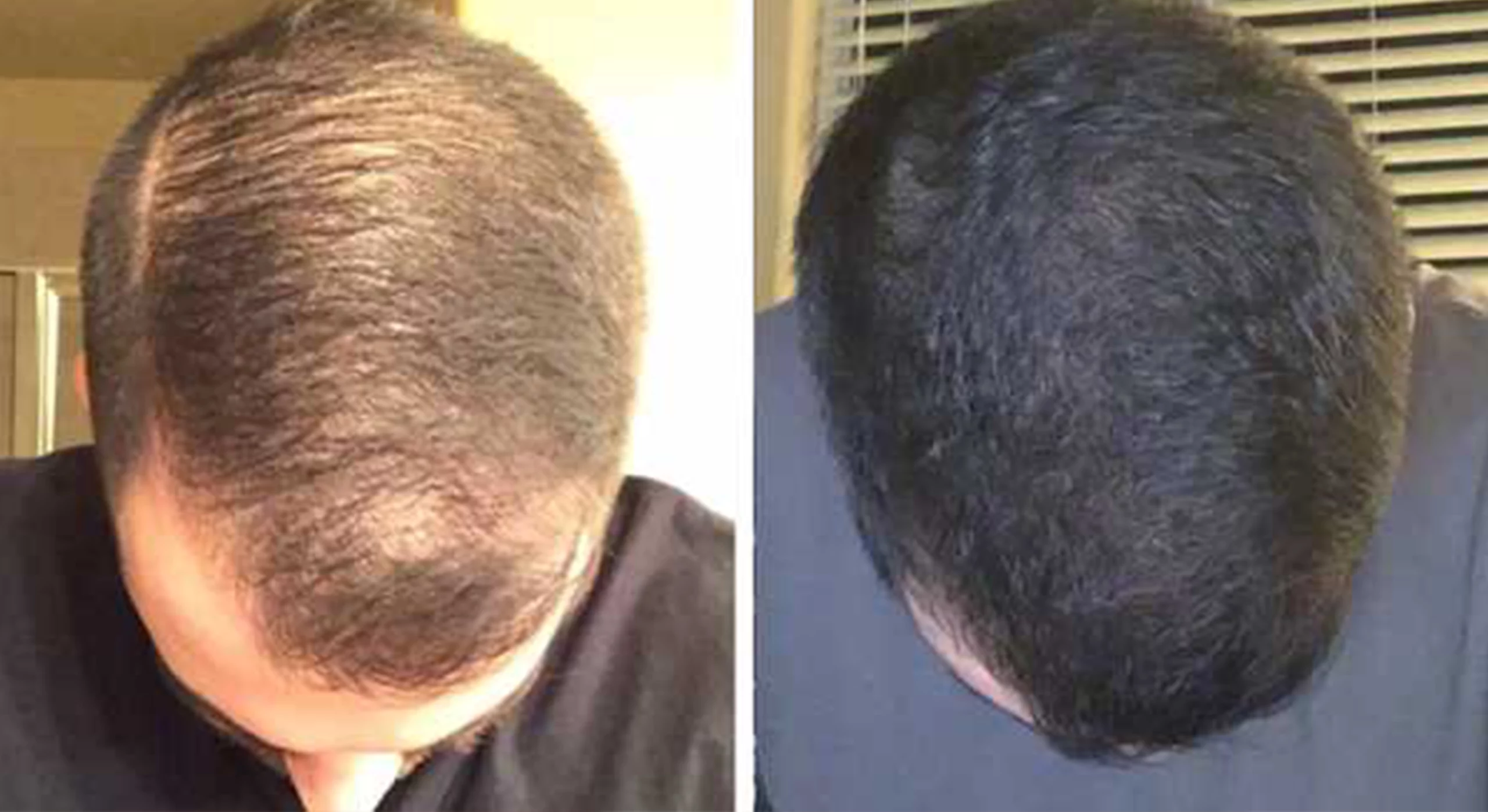
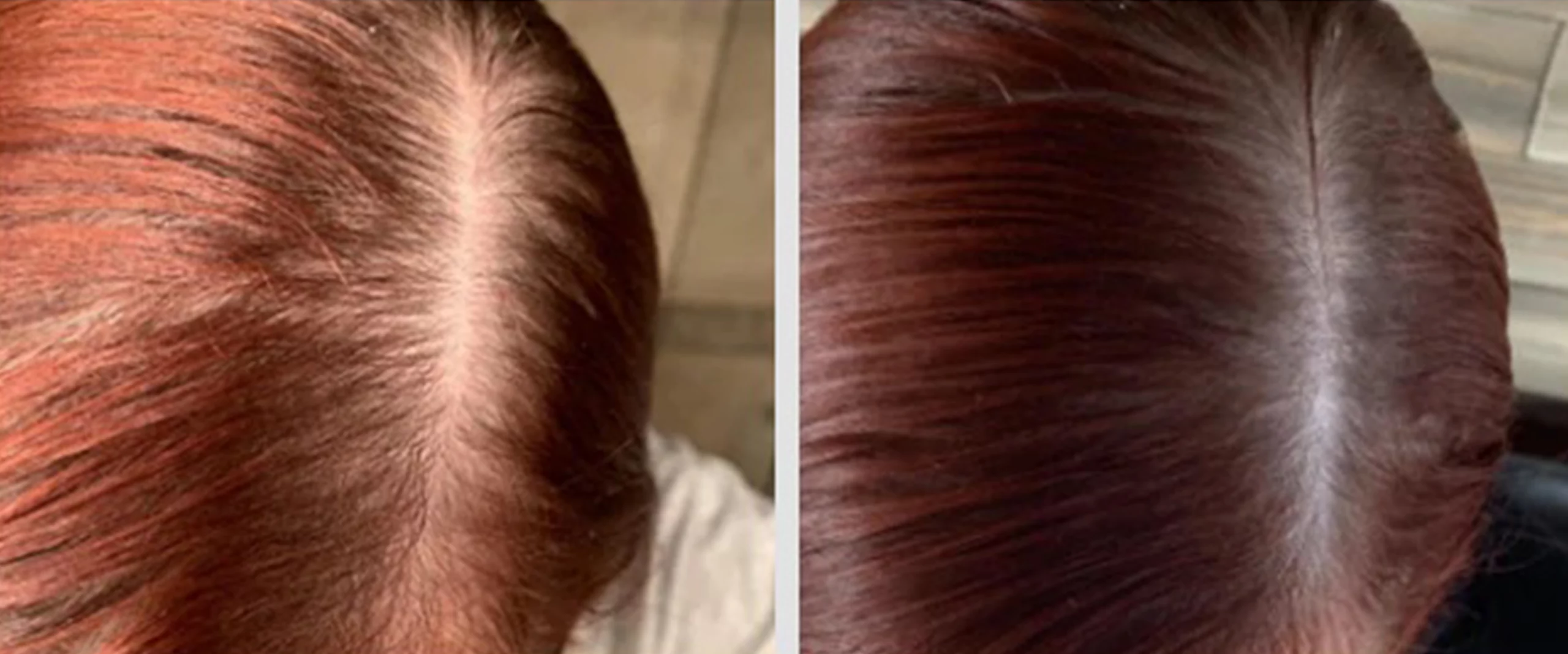
FAQs
What is frontal fibrosing alopecia?
Frontal fibrosing alopecia is considered a scarring hair loss condition that happens when inflammation is causing damage to the hair follicles. It is usually more seen in the frontal hairline of the scalp but could also be found in other areas such as the eyebrows.
Frontal fibrosing alopecia can happen to anyone, but dermatologists typically see it in postmenopausal women above 50 years old.
The condition is seen as a variant of lichen planopilaris, which is also a scarring hair loss problem, because of their similarities in the skin biopsy test, but there are still some differences that make some dermatologists disagree.
What causes frontal fibrosing alopecia?
There are many triggers to frontal fibrosing alopecia, but there is no apparent cause. Some of the triggers are:
- Genetic reasons/ family history: although it is not a hereditary disease, frontal fibrosing alopecia is reported to affect people from the same family.
- Hormonal: mostly found in postmenopausal women because of hormonal changes. Also, thyroid problems might get you frontal fibrosing alopecia.
- Autoimmune: some autoimmune diseases like lupus erythematosus and rheumatoid arthritis could be triggers.
- Inflammatory: the lymphocytes, which are part of immunity that initiate inflammation, cause inflammation due to the attack on the hair follicles.
- environmental factors: like sun exposure or sunscreen ingredients, and dietary factors
- Contact allergy: allergies of hair products like dyes, creams, oils, fragrances, etc…
Inflammatory cells called lymphocytes, which are part of the immune system, attack the hair follicles. This causes inflammation and scarring and leads to hair loss. Treatments are aimed at halting inflammation.
What are the symptoms of frontal fibrosing alopecia?
The main symptom of frontal fibrosing alopecia is hair loss and scarring in the frontal area of the scalp. The band of hair loss on the front and sides of the scalp is usually symmetrical and slowly receding over time.
Frontal fibrosing alopecia may have no symptoms other than hair loss or appear as an itchy, painful, or burning sensation with redness in a band across the hairline in the frontal area of the scalp. After that, the skin will start looking pale, flaky, shiny, or mildly scarred, without visible hair follicle openings.
Eyebrow thinning or loss (madarosis) is also a common symptom that can happen prior to hair loss of the scalp. Many areas in the body can be also affected by hair loss.
The hair loss rate can vary from one to another, but it causes the frontal hairline to increasingly recede over time. Once the hair loss happens, it will not re-grow in this area.
How do dermatologists diagnose frontal fibrosing alopecia?
Most dermatologists can diagnose FFA clinically. If in doubt, a skin biopsy is used to confirm frontal fibrosing alopecia. A small sample of the area affected is taken and tested under the microscope. Your dermatologist will see the inflammation and scarring signs.
Blood tests are also recommended to check the hormonal levels (eg. thyroid hormones).
Frontal fibrosing alopecia can sometimes be missed due to similar cases including:
- Androgenic alopecia (both in males & females): which is caused mainly due to hormonal disturbance.
- Traction alopecia: which is a hair loss condition that’s caused by repeatedly pulling on your hair.
The Lonely hair sign, which is a hair loss pattern that gives the illusion of having only one hair in the affected area, is noticed by the dermatologist
Skin colour difference: a difference of colour is noticed between the area which had hair follicles before and the skin of the face. The hypopigmentation is better seen by Wood’s lamp, which is a diagnosing tool.
What is the treatment used in frontal fibrosing alopecia?
There is no current treatment for frontal fibrosing alopecia till now, but since inflammation is involved, dermatologists prescribe anti-inflammatory drugs to decrease the hair loss progression.
Frontal fibrosing alopecia can be more manageable in the inflammatory phase, where there are still working hair follicles. After inflammation subside, the hair follicles start to develop a smooth shiny appearance. This signifies end stage scarring FFA, hair regrowth at that stage is unlikely to occur.
Some of the treatment options are:
- Topical corticosteroids: steroids can be found in the form of gels, lotions, or creams. They are applied to the skin on the front of the scalp. Steroids are also used with treatment, as they may not be effective alone to decrease hair loss.
- Topical Tacrolimus: it is a topical ointment or cream that acts by suppressing the immune system and managing the inflammation where it is applied.
- Intralesional steroids. Dermatologists inject steroids into the affected skin to manage the inflammation, thus decreasing hair loss. This treatment may need to be repeated to get the best results.
- Antibiotics e.g., tetracycline, doxycycline. These medications are used here to help in minimizing inflammation and redness, but not for their antibiotic effect.
- Hydroxychloroquine: which is typically used as an antimalarial drug, stops frontal fibrosing alopecia in some people. It takes time to work and also comes with serious side effects, so consult your doctor before taking any medicine.
- Immunomodulatory drugs e.g., mycophenolate mofetil. These can help to suppress the immune system and prevent inflammation around the hair follicles. In some people, it can slow or stop hair loss, but they are rarely used due to the side effects.
- Antiandrogen treatments e.g., oral finasteride and dutasteride. These treatments work by maintaining normal levels of testosterone (which is naturally found in both men and women) in the hair follicles.
- Rituxomab and adalimumab: they are novel new treatments used in many conditions and used to decrease inflammation.
- Hair graft: hair transplantation is used when the inflammation stops and the hair loss is stopped.
Most dermatologists will recommend a combination treatment as it gives the best results. The earlier the treatment starts, the better the hair responds to the treatment.
Support groups also can make it easier to deal with and adjust with frontal fibrosing alopecia. Wigs can also be an option for people who are not comfortable with their looks.
What are other novel treatments?
Lasers, LLED, microneedling & PRP have all been reported in the literature. The maybe considered as adjunctive therapies. Our dermatologist will guide you.
What can you do to help with hair loss?
Some self-care tips also include:
- Be gentle with your skin. Frontal fibrosing alopecia causes inflammation. Try being gentle when handling the hair loss-affected areas to avoid more inflammation. This means washing your face (and other areas) gently with your fingertips.
- Use a mild, fragrance-free cleanser in the hair loss area.
Avoid any hairstyling tools or chemicals. This can speed up or cause more inflammation to your hair, leading to more hair loss.
What is the outlook?
Frontal fibrosing alopecia is usually progressive, and the hairline can recede to almost 2.6 cm. However, hair loss slows down & eventually stabilises over a period of 3-6 years.
This condition is challenging as the problem may get missed and not recognized until the hair loss has progressed. Dermatologists’ efforts in diagnosis and disease stabilization generally take months to years, and recurrence is quite common.




