Lichen planopilaris is an inflammatory condition that results in permanent & progressive hair loss. It is often found more in adult women but can be found in both gender and any age group. It is thought to be an autoimmune disorder and the most common symptoms can be redness, scaly scalp, pain, and/or itchiness. Anti-inflammatory medications are sometimes useful to halt hair loss in lichen planopilaris.
Key Points
- Lichen planopilaris is an inflammatory condition that leads to permanent hair loss
- The cause of lichen planopilaris is autoimmune
- The symptoms may include redness, itchiness, and/or pain
- Anti-inflammatory drugs can decrease the symptoms & slow hair loss
- Early treatment is critical to prevent further hair loss
Lichen Planopilaris at a glance
Our results speak for themselves
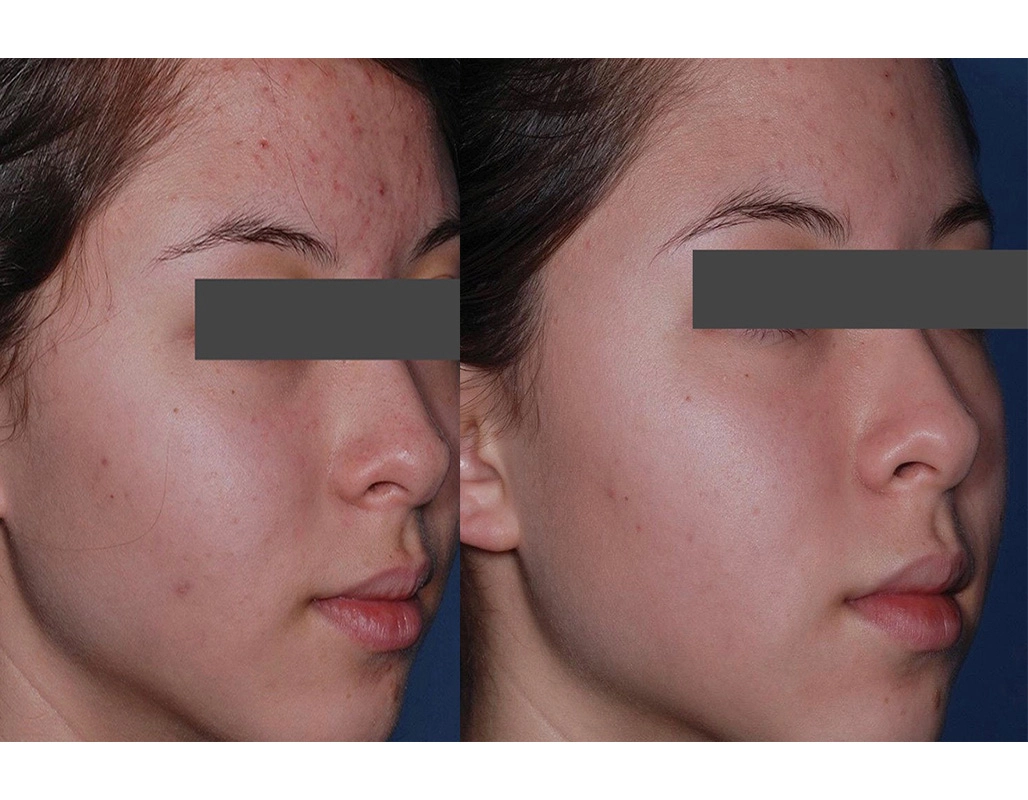
Before
After
Obagi has medical grade therapy for acne. Benzoyl peroxide combined with active wash, cleanser & moisturizer
Ask us more about this treatmant
Preferred Consultation
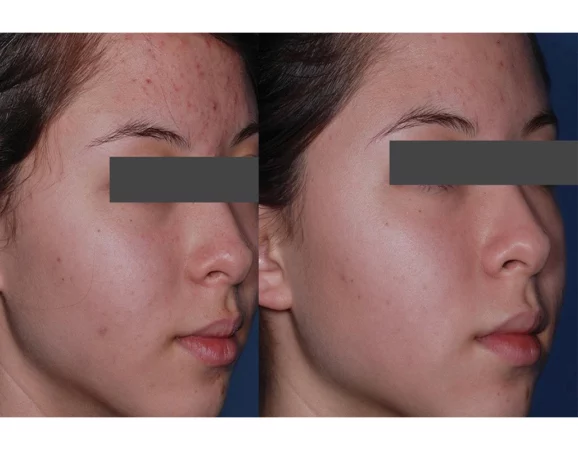
Before
After
Medical therapy for acne
Ask us more about this treatmant
Preferred Consultation
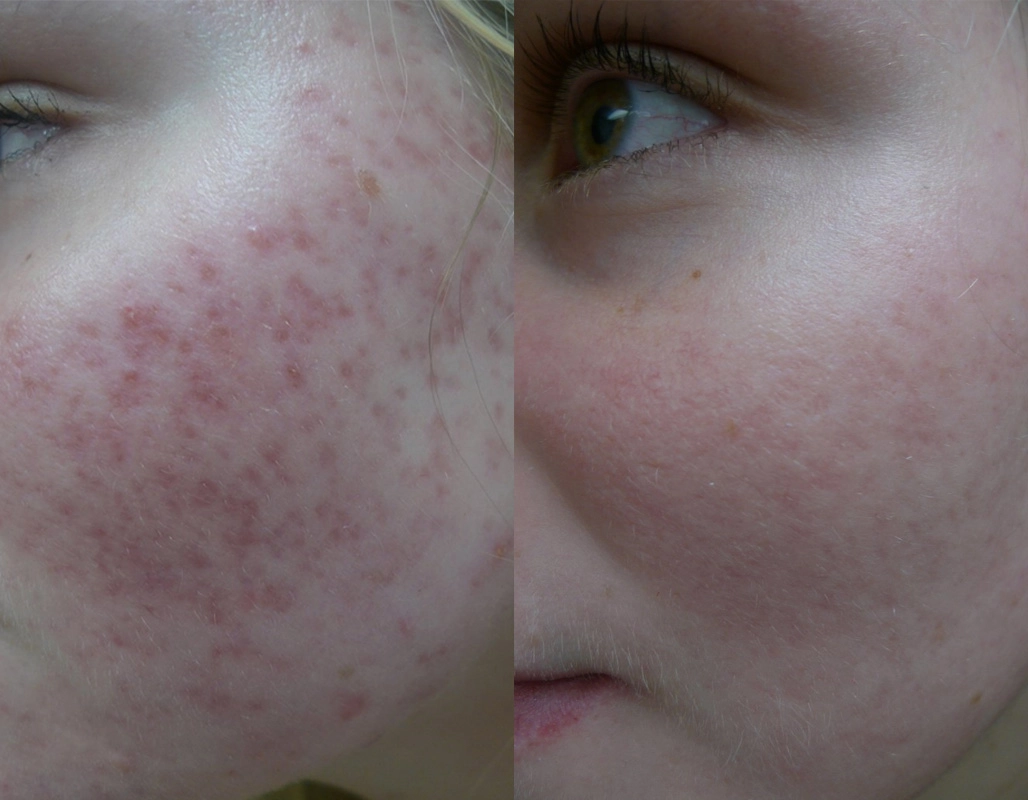
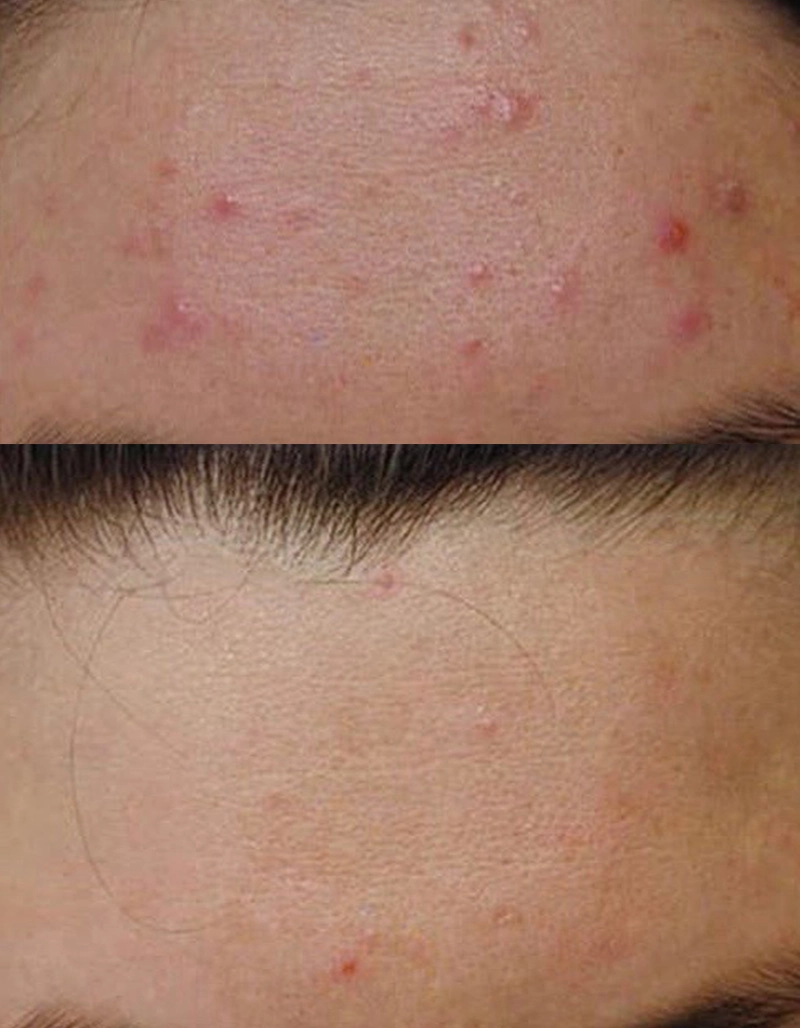
Before
After
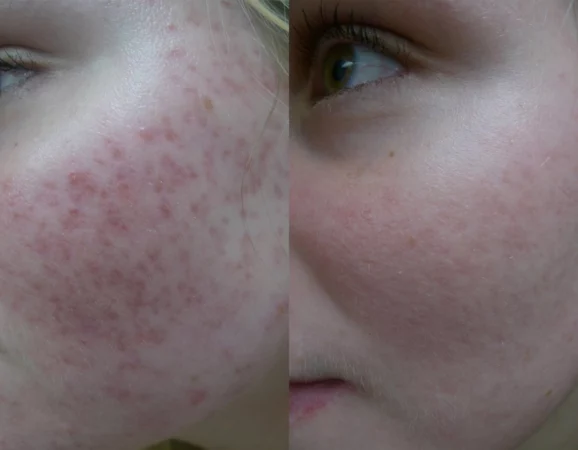
Topicals to treat acne, vascular laser therapy to reduce redness
Ask us more about this treatmant
Preferred Consultation
FAQs
What is lichen planopilaris?
Lichen planopilaris is a permanent hair loss condition that results from progressive inflammation & scarring. It is a rare condition, but it is the most common cause of scarring hair loss of the scalp. This condition is more likely to be seen in adult women than men, and it is not contagious.
Lichen planopilaris is a form of lichen planus, an inflammatory disease that affects the mucous membrane and skin. While the main symptom is hair loss, lichen planopilaris may also cause redness, itching, and pain in the follicles.
Lichen planopilaris has three variants that differ in the location of the symptoms:
- Classic lichen planopilaris, also known as follicular lichen planus
- Frontal fibrosing alopecia (FFA)
- Graham-Little-Piccardi-Lasseur syndrome (Graham-Little syndrome, GLPLS)
Why treats this at Cutis Dermatology?
Our hair experts include Dr Esh & Dr Heba. They have extensive experience in treating all forms of lichen planopilaris, including frontal fibrosing alopecia.
What causes lichen planopilaris?
The cause of lichen planopilaris is unknown, but it is thought to be an autoimmune disorder where the T-lymphocytes, a type of white blood cell, are attacking the hair follicles resulting in inflammation.
Although lichen planopilaris is not hereditary, some genes related to the immune system could be responsible for increasing the possibility of having this condition.
What are the symptoms of lichen planopilaris?
Classic lichen planopilaris symptoms may vary from person to person in their severity, & some don’t experience all or any of the symptoms.
While the main symptom of lichen planopilaris is progressive hair loss, other symptoms include:
- Scalp itchiness
- Scalp redness
- Pain or discomfort felt in the affected area
- Tenderness
- Burning
What does the scalp look like?
Lichen planopilaris typically appears as redness & scaling of the skin around the base of a hair and blocking of the hair follicle, which can make the scalp have a rough texture.
The area of hair loss appears smooth & shiny & has no visible hair follicles. It happens in the front, lower, or side areas of the scalp and can occur in small focal areas which can later merge into bigger ones. Lichen planopilaris can also involve other areas like facial and body hair.
What variants of lichen planopilaris are there?
Other variants of lichen planopilaris are:
- Frontal fibrosing alopecia: commonly affect postmenopausal women, usually in the frontal area of the scalp. It also causes scarring, & the hair loss is permanent. It can be accompanied by hair loss of eyebrows as well.
- Graham Little Syndrome (Piccardi-Lasseur-Graham Little Syndrome): This syndrome is similar to lichen planopilaris in the patchy hair loss in the scalp, but it also comes with hair loss in the armpits and pubic area. Itchy rash and bumps are also sometimes found in Graham Little syndrome.
Products

O Cosmedics cleansing range
$63.00-$64.00

O Biotics 3D Hyaluronic Serum
From $97.00
Our dermatologists are experts in the management of common & rare causes of hair loss, including lichen planopilaris & frontal fibrosing alopecia. With inflammatory disorders of the scalp, early & effective treatment preserves the remaining follicles.
How is lichen planopilaris diagnosed?
The diagnosis of lichen planopilaris is often made with a clinical examination of the affected area. Dermatologists may also run a microscopic examination to verify lichen planopilaris.
Your dermatologist will take a biopsy of a skin that includes hairs with surrounding redness and scale at the edge, as an already scarred area of hair loss will not help confirm the diagnosis.
How can lichen planopilaris be treated?
Lichen planopilaris’s primary aim of treatment is to stop the progression of hair loss and save the remaining hair. In some cases, the hair loss can eventually stop by itself, but since the hair loss is permanent, dermatologists recommend early management to avoid losing a lot of hair.
What are the lifestyle options?
Hair loss can be a painful emotional experience, that’s why some doctors recommend going to hair loss support groups to cope better. Wigs and hairpieces are also options available
What is the outlook of the lichen planopilaris?
Lichen planopilaris may ‘burn out’ after a period of years. Early management is important to preserve remaining hair follicles.
Your dermatologist will give you regular follow ups to assess & prevent further hair loss.


