Ota birthmarks, also known as naevus of Ota, are common birthmarks treated at Cutis Dermatology, Brisbane. This type of birthmark is more common in women of Asian descent. Ota birthmarks are due to increased pigment cells known as melanocytes in the dermal layer of skin. It mainly affects the face and gives a grey-blue or brown color. Laser treatment is very successful in permanently removing Ota marks.
Key Points
- Ota birthmarks are hyperpigmentation caused by pigment in the deep layer of skin
- The color of the affected skin is grey to blue, frequently involving the eye area
- Ota birthmarks can be treated with laser therapy
- Ota birthmarks are usually benign, and their effects limit only to the physical appearance
- Most cases require 4-9 sessions, spaced 7-12 weeks apart
- The best laser to date is Picoway by Candela
- Complications of Ota birthmarks can include glaucoma
Ota Birthmarks at a glance
Our results speak for themselves
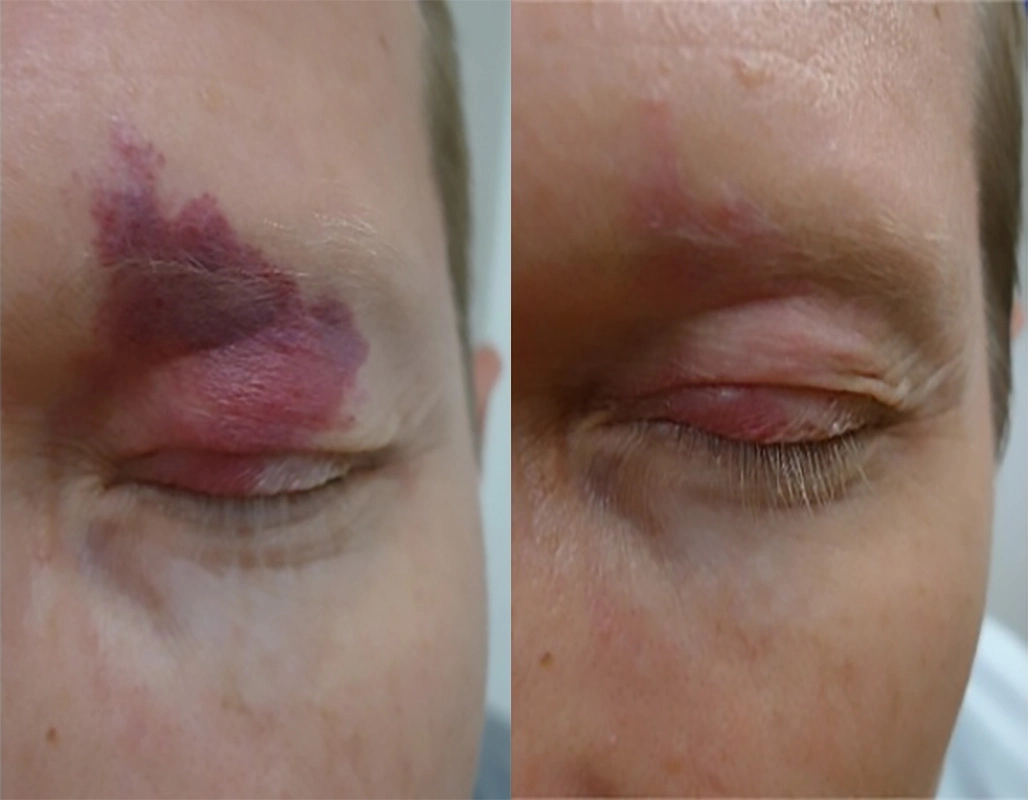
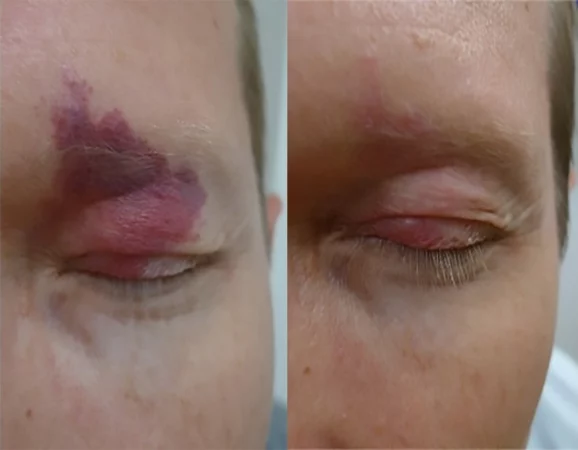
VBeam for port wine stain. 3 sessions. The
number of treatments range from 2-15,
depending on site, & extent
Ask us more about this treatmant
Preferred Consultation
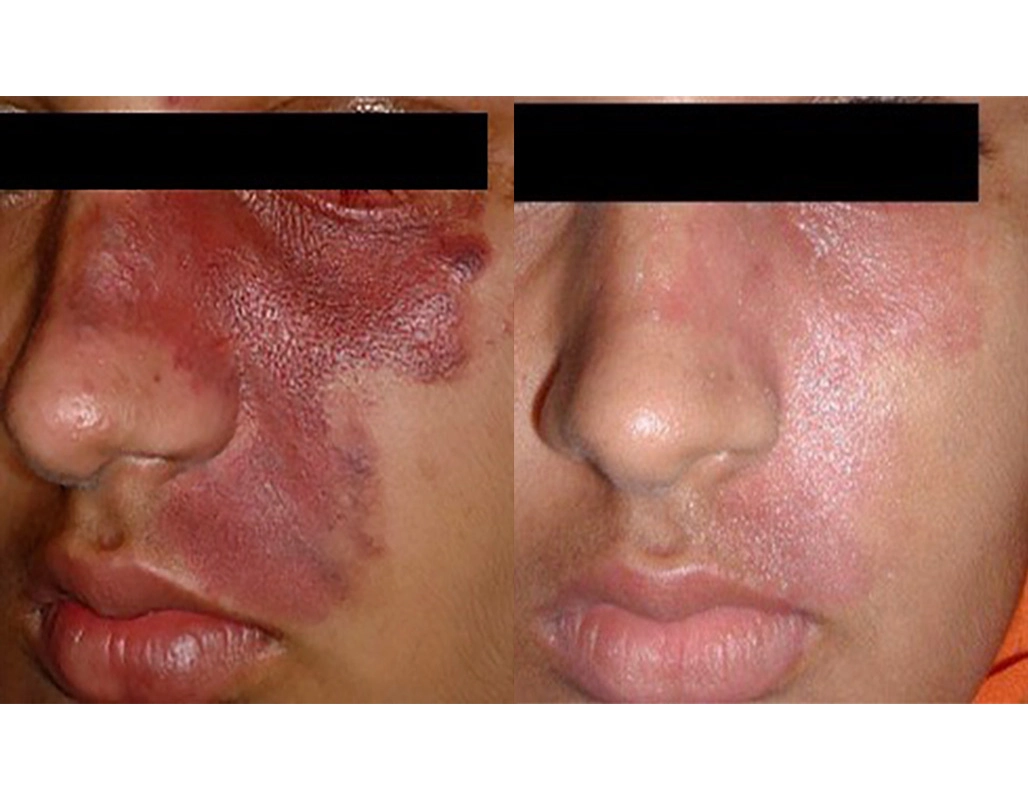
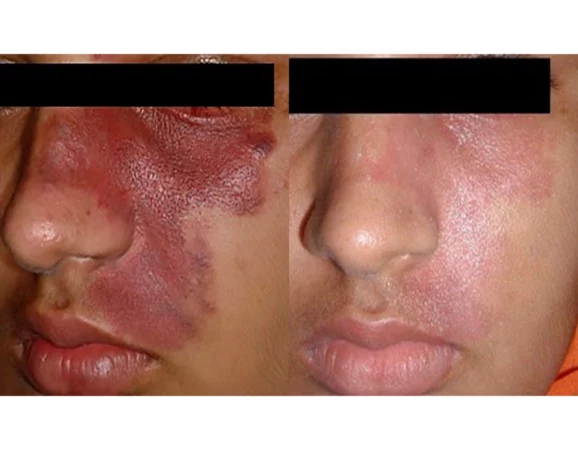
Vascular laser for port wine stain
Ask us more about this treatmant
Preferred Consultation
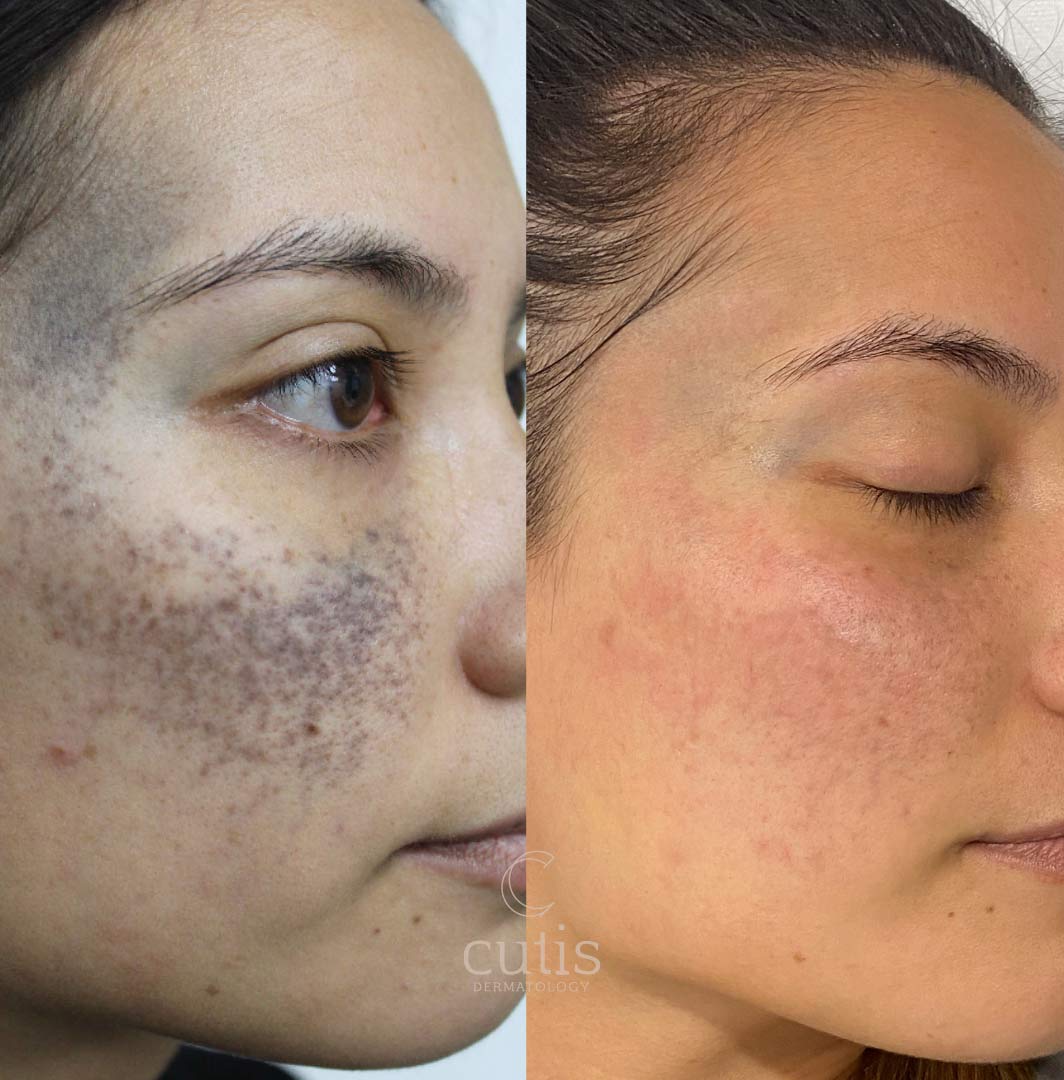
Pico lasers can effectively remove deep pigment including Ota birthmarks. 4-6 sessions.
Ask us more about this treatmant
Preferred Consultation
FAQs
What is an Ota birthmark?
The Ota birthmark, also known as the naevus of Ota, is considered hyperpigmentation found on the eye and/or the surrounding skin tissue of the eye and face. It is caused by excessive and abnormal melanocytes’ collection in the upper dermis layer of the skin, which are responsible for skin pigmentation. The birthmark tends to have a bluish or brownish color.
Cutis Dermatology, Brisbane, treats over 150 cases of Ota a year. It is more common in women of Asian descent.
How do we treat Ota birthmarks?
There are different treatment approaches for Ota birthmarks, and your dermatologist can help you explore all the best options to take.
Options can include cosmetic covers to help camouflage the pigment, however lasers offer the best solution.
How is laser therapy used in Ota birthmarks?
Laser therapy may be the most effective option, as its mechanism of action is to destroy the excess dermal melanocytes that cause bluish/brown hyperpigmentation. Laser devices like picosecond lasers are considered very effective. However, laser therapy needs multiple treatments with a combination of devices and applications.
Once treated Ota hyperpigmentation doesn’t return.
What are the best lasers for Ota birthmarks?
To date, the best laser is a pico laser, namely Picoway. Pico lasers give a marginally faster response compared to old nano QSL Nd:YAG laser, however their complication rates are much less.
Historically ruby lasers and alex lasers have been used to treat Ota naevi. Cutis is currently involved in a study using short PD nano lasers compared to pico. Studies will be complete in late 2023.
How many sessions of laser will it take to treat Ota birthmarks?
Ota will respond within 1-2 sessions. This enables the patient to better camouflage with make-up. For optimal outcomes, between 4-10 sessions are required. Laser treatments are spaced between 7 to 14 weeks apart.
Will Ota recur following laser treatment?
Recurrence is unlikely following removal of melanocytes & pigment. The caveat is that if there are residual pigment cells, sun exposure can awaken the dormant pigment cells, leading to increased pigmentation.
How long does it take to recover from laser treatment?
Bruising and scabbing will take around a week to resolve. There may be some short-lived skin colour changes that may last 4-8 weeks. It is important not to get sun-exposure after your laser for 4 weeks.
Is treatment painful?
Yes, hence why we use numbing gel. In some cases, we also use numbing injections to ensure that treatments are comfortable.
What are the side effects of lasers?
Side effects are rare since using the latest pico laser. Side effects are different compared to expected outcomes (bruising, scabs, transient skin colour changes).
Prolonged side effects are rare (less than 2% of cases) and include, hyper (darkening) or hypo (whitening) pigmentation of the skin. Scarring was more commonly seen with ruby and Alex lasers (more than 20 years ago). Individuals with naturally darker skin are more complicated to treat, as their treatment can result in prolonged skin colour changes.
Does Medicare cover treatment?
Medicare partially covers treatment of Ota birthmarks. Up to 6 sessions are subsidized per calendar year.
This type of birthmark is more common in women of Asian descent. Ota birthmarks are due to increased pigment cells known as melanocytes in the dermal layer of skin. It mainly affects the face and gives a grey-blue or brown color. Laser treatment is very successful in permanently removing Ota marks.
What are the causes of Ota birthmarks?
There are no definitive causes of Ota birthmarks. This condition can be linked to a genetic mutation.
Melanocytes are found entrapped in the upper third of the dermis layer in the skin of the face. It is usually unilateral, meaning only one side is involved. Most Ota birthmarks affect the sclera of the eye, increasing the risk of glaucoma.
Ota birthmarks are five times more likely to be found in women than in men. Furthermore, ethnicity also plays a part in getting Ota birthmarks, as Asians have a higher prevalence rate than Caucasians or Africans. Nevertheless, anyone can have ota birthmarks.
Almost half of the cases are congenital, but it can happen at puberty as well.
What other conditions can look like Ota birthmarks?
Some cases who experience hyperpigmentation on their face may have a condition called melasma. This affects both sides of the face, unlike Ota. Melasma can be associated with-
- -Pregnancy
- -Hormonal changes
- -UV light
- -Thyroid problems
- -Medications like hormonal and contraceptives
Other than melasma, there are different conditions that can cause blue or grey discoloration in the face like –
- Hori naevi, this is more common than Ota & is more discrete.
- Drug-induced pigmentation, most often due to minocycline
- Post inflammatory pigmentation
- Lichen planus pigmentosus & ashy dermatosis
What do Ota birthmarks look like?
Ota birthmarks are hyperpigmentation that appear blue/grey, or brown and, in most cases, involve only one side of the face, which is called unilaterally but can be present bilaterally on both sides of the face.
Hyperpigmentation is found on the face and around the eyes. You can see Ota birthmarks on the eyelids, nose, forehead, cheeks, whites of the eye, and/or irises. These parts of the face are controlled by the trigeminal nerve, which is responsible for facial sensation.
Ota birthmarks that appear around the eye seem to have thicker tissue skin around and in the eye. The color of it can transition from light to dark through age, but the spot doesn’t spread or diffuse away from the trigeminal nerve-controlled area. Ota birthmarks are not a contagious condition.
How do dermatologists diagnose Ota birthmarks?
Dermatologists depend on their diagnosis of Ota birthmarks mainly on the appearance of the discoloration on the face. They also may take a small biopsy of the hyperpigmented area to confirm the increased melanocytes in the skin.
When the discoloration is in the eye, the ophthalmologist will examine it much further by using a biomicroscope or ophthalmoscope. Some cases may even require an ultrasound of the eyes.
There are also cases that may have hyperpigmentation in places besides the usual areas typically affected by Ota birthmarks, which dermatologists will further investigate, like nevus of Ito, a condition that causes hyperpigmentation of the arms, shoulders, underarm, and neck.
If you experience any discoloration on your skin near your eyes or in them, see your dermatologist to observe and give you the best treatment plan for your case.
What is the cosmetic approach in Ota birthmarks?
The cosmetic approach to Ota birthmarks helps many cases to cover the discoloration, by using multiple techniques like camouflaging creams, foundation, concealers, or any color correcting products to conceal the lesions.
In most cases, one to two laser sessions will enable patients to effectively cover up Ota birthmarks.
Can Ota birthmarks cause complications?
Ota birthmarks may have some serious complications, especially if the eye is affected. Ota birthmarks in the eye can lead to glaucoma as some doctors believe the melanocytes interfere and block the flow of fluids in the eye, leading to an increase in eye pressure. Your doctor will plan regular check-ups on your eye to avoid complications.
Ota birthmarks could also be a cause of malignant melanoma, which is a fatal and life-threatening complication in most cases. A regular check-up is also advised.
Recurrence is also a common problem in Ota birthmarks when the lesions are not completely removed.
Psychological issues like low self-esteem and depression may also be a problem due to Ota birthmarks and, in some cases, may need psychological help from therapists.
What are other spectrums of dermal melanocytosis?
The dermal melanocytic spectrum includes-
- Naevus of Ota: which is found on the forehead and face around the eye area. Discoloration of parts of the eye may occur (sclera, cornea, iris, retina)
- Naevus of Hori: it is a condition like naevus of Ota but affects both sides of the face, bilaterally. Hori naevi are very common in Asian women. We treat 1-2 Hori daily at Cutis Dermatology, Brisbane.
- Naevus of Ito: it is mainly seen on the shoulder and upper arm area (shoulder girdle).
- Mongolian blue spot is frequently seen in Asian newborns. They are self-limiting
- Unclassified deep dermal melanocytois of Asians not related to Hori naevi. This controversial entity is frequently seen in Asian women.
About half of the birthmark cases are born with it, while the rest of the cases develop it in adolescence. It is five times more common in women than in men.
What’s the outlook for Ota birthmarks?
Ota birthmarks mostly remain unchanged and permanent through the years without treatment, but the lesions can be treated by laser or other options if wanted.
Further pigmentation to Ota birthmarks can happen when there is excessive sun exposure, and wearing sunscreen is very essential in these cases. Regular check-ups with your dermatologist are recommended.
Ota birthmark lesions are mostly benign, and their effects are mostly on the physical appearance.




