Hormones can play a significant role in the development of acne. PCOS or polycystic ovarian syndrome is the most common cause of hormonal acne. It affects one in fifteen Australian women. This form of acne usually requires specialist intervention.
Key Points
- PCOS can lead to acne, most commonly on the jawline & neck
- This form of acne frequently leads to scarring as cysts are deep
- Topicals creams are rarely effective
- Effective treatments are possible
- Dermatologists employ peels, lasers, & hormonal control to treat PCOS associated acne
PCOS & Acne at a glance
Our results speak for themselves
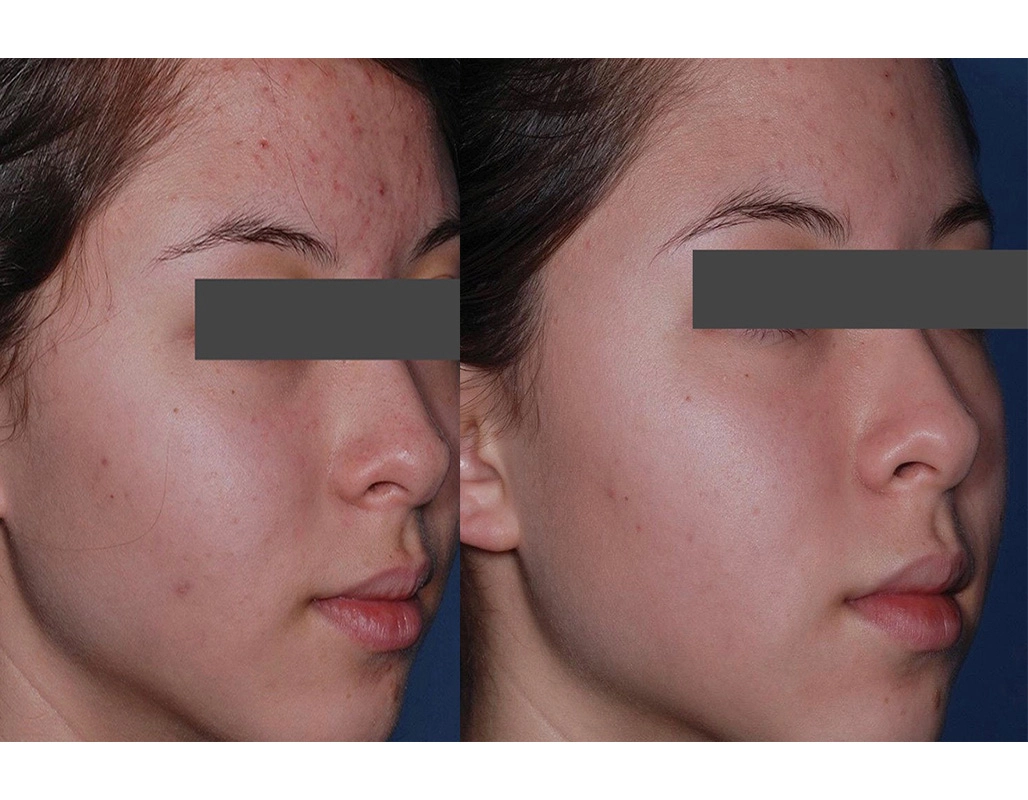
Before
After
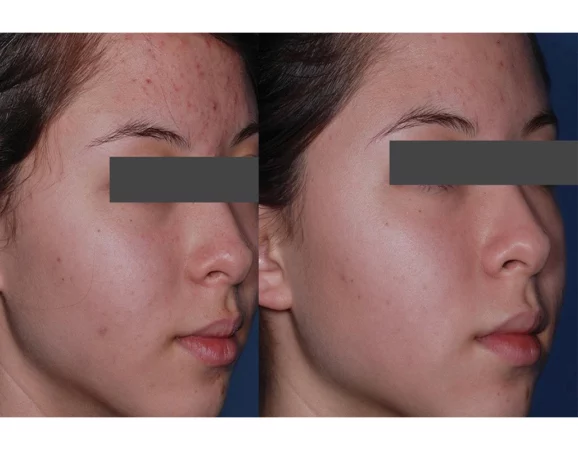
Obagi has medical grade therapy for acne. Benzoyl peroxide combined with active wash, cleanser & moisturizer
Ask us more about this treatmant
Preferred Consultation
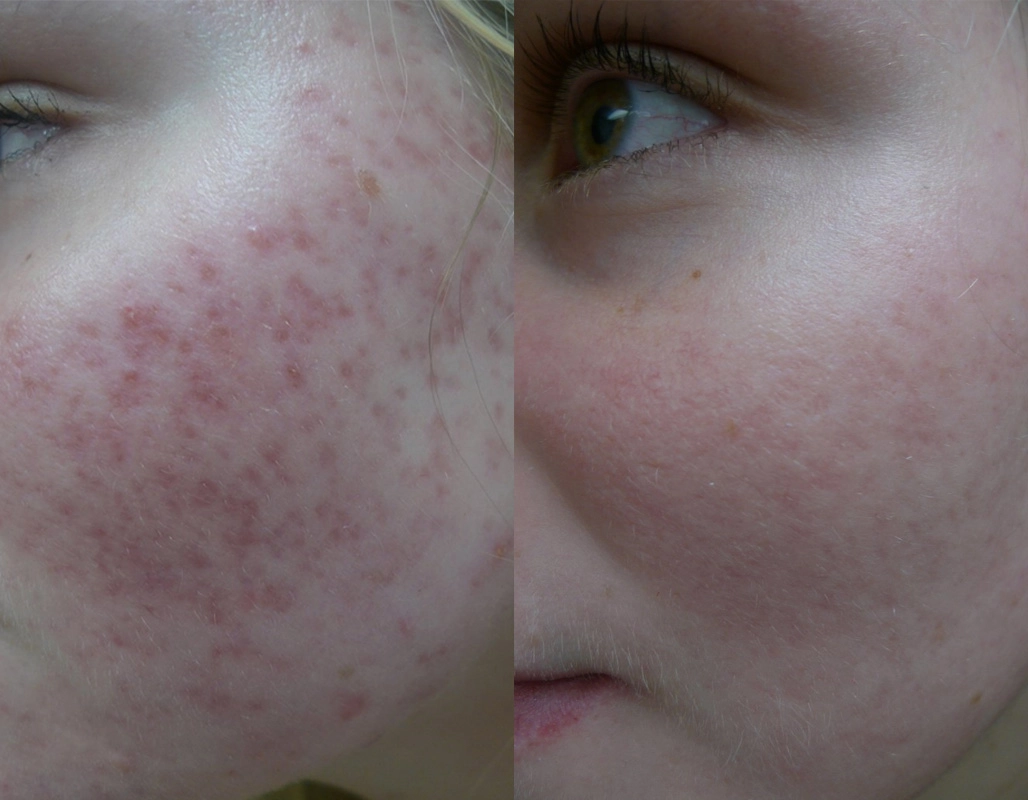
Before
After
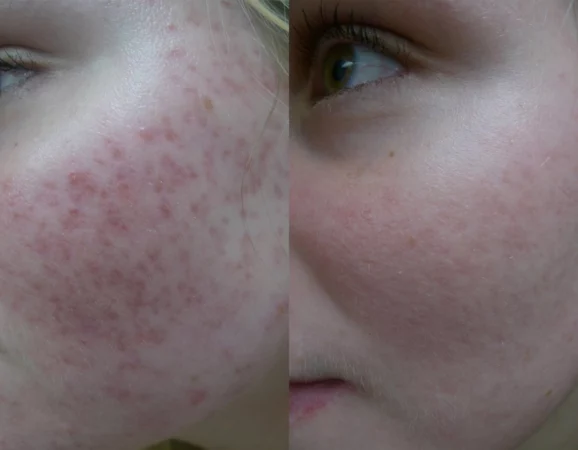
Topicals to treat acne, vascular laser therapy to reduce redness
Ask us more about this treatmant
Preferred Consultation
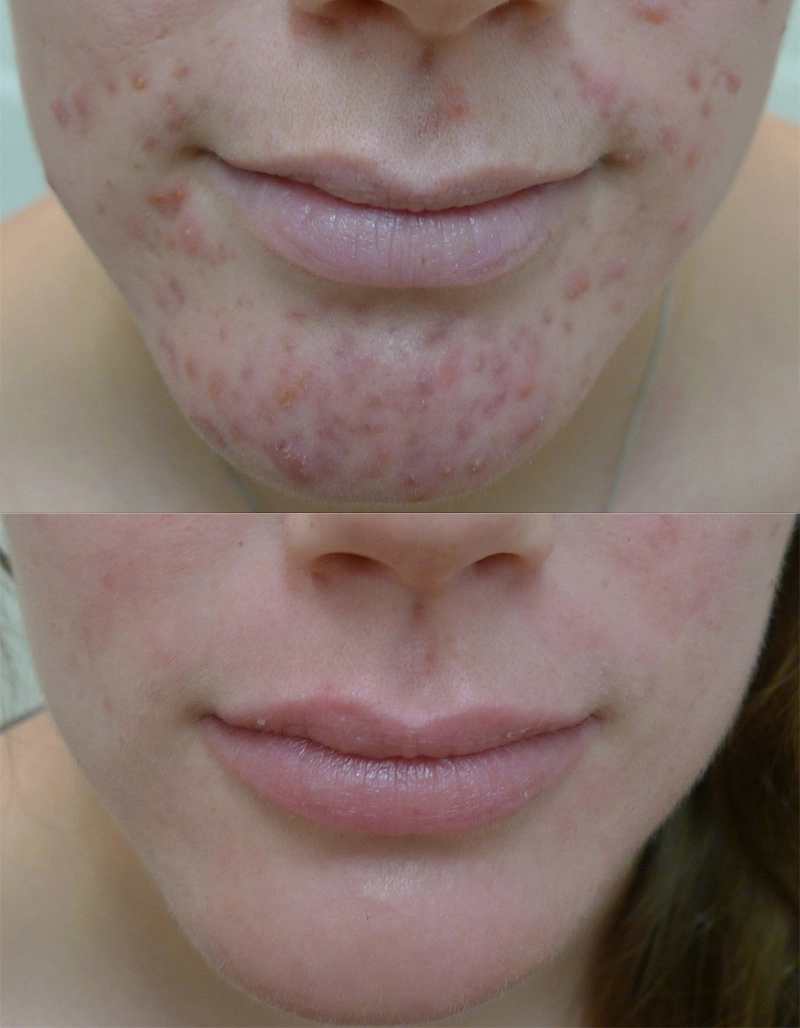
Before
After
Hormonal control & vitamin A
Ask us more about this treatmant
Preferred Consultation
FAQs
What is PCOS?
PCOS or polycystic ovarian syndrome is a common cause of hormonal acne. Skin changes of PCOS include acne, excessive hair growth, hair loss, oily skin, tags, & pigmentation.
PCOS can also lead to weight gain, infertility, period changes, as well as metabolic abnormalities such as glucose intolerance.
How is PCOS acne different?
PCOS acne falls under the blanket term of ‘hormonal acne’. This type of acne presents differently in comparison to teenage or T zone acne. PCOS acne can affect the jawline and neck area. In many cases it can extend to the trunk. Deep cysts are frequently seen in hormonal acne.
As this type of acne is deep, it often requires specialist treatment to shift. Unlike normal acne, PCOS acne frequently scars– hence the importance of early management.
What can you try at home before seeing a dermatologist?
Try this, it can be helpful in some cases of PCOS acne.
AM: Salicylic acid washes, followed by topical vitamin B
PM: As above with washes, add high strength retinol
Lifestyle choices are super important, including an anti-acne diet, exercise, weight management & good makeup practices. It takes 8 to 12 weeks for DIY skin care to work, so be patient.
How do dermatologists treat PCOS related acne?
Acne in PCOS can be resistant & persistent to normal therapy, including topical skin care. Our dermatologists can prescribe:
- Antihormonal tablets
- Topical retinoids
- Oral retinoids
- Chemical peels including retinoic acid or salicylic acid
- Laser light treatments such as Kleresca, LEDs, & blue light BBL
Perform extractions for deep cysts, most frequently around the jawline area
How to I prevent acne from scarring?
Mitigation is the key. Treat acne early & effectively. Don’t pick. Use acne patches (see the section on skin care for acne).
Our team employs pico lasers, Tixel resurfacing as well as vascular & fractional lasers to effectively treat scars. Book a FREE consultation with your nurses.
What can be done about excess hair or hirsutism in PCOS?
Excess hair is frequently seen in PCOS patients and is due to excess androgens or male hormones. Effective treatments that we employ include laser hair removal using the 1064 hair removal laser by Lumenis.
Antiandrogens can also reduce unwanted hair.
PCOS is a common cause of chronic adult female acne. It is often associated with acne scarring. Our dermatologists can implement a safe & effective treatment regime to reduce outbreaks & promptly repair acne scars.
What about hair loss?
Hair loss can occur in PCOS. This can be treated with antiandrogens as well as minoxidil topically or systemically. Growth factor injections and light therapy can be useful.
Book an appointment with our dermatologist for effective solutions
How to treat dark patches or acanthosis nigricans?
Dark patches are frequently seen in PCOS patients and can be located on the neck, underarms, groin and occasional on the face. This condition is termed acanthosis nigricans.
Treatment options include-
-
- Topical retinoids such as tretinoin (retinol is too weak)
- Lasers such as pico
- Hormonal control
- Metformin
- Exfoliants such as glycolic, salicylic and lactic acids
What is metformin and how is it used in PCOS patients?
Metformin is a drug used to modulate IGF or insulin levels. This tablet can treat skin associated with PCOS, in addition to reducing visceral and body fat. It can be prescribed by endocrinologists, GPs & dermatologists.
Though controversial, metformin is also prescribed for longevity and anti-aging, in conjunction with resveratrol & other antioxidants. There is some evidence that it can reduce acne, however it is best used as part of a treatment plan, and not monotherapy.
What are lifestyle and DIY home treatments for PCOS?
The biggest gains from DIY treatments include-
- Diet. This improves blood sugar levels and can also significantly improve acne. Consume organic foods, low in sugar, high in complex carbohydrates and protein. Omit all dairy products including milk, yogurt and cheese.
- Skin care includes high strength retinol and azelaic acid. The latter can also improve post-inflammatory hyperpigmentation seen after active acne.
- Makeup choices and best practices. Mineral over oil-based foundations. Remember to have at least two make-up free days to let your skin breathe.
- Supplements include zinc sulphate. This can help reduce acne & inflammation.
- Exercise & weight management will improve your skin.
What tests are there for PCOS?
There are strict diagnostic criteria for PCOS. Be guided by your healthcare provider.
PCOS can be labelled if there are two out of three of the following-
- Physical or biochemical signs of androgen excess, namely acne, hair loss, hirsutism.
- Ovulatory problems, such as heavy bleeding or irregular bleeding.
- Polycystic ovaries on ultrasound with cysts less than 9mm but more than 2 mm or total ovarian volume of 10ml or more.
Can you still have PCOS with normal hormonal tests?
Yes. Remember that blood tests only form one out of the three criteria for PCOS. You may have normal levels of androgens in the blood, however an abnormally high concentration in the skin.
Alternatively, your oil gland & hair follicle may be more sensitive to normal hormones. This is referred to as an intracrine dysfunction.
Who should be involved in treating PCOS?
PCOS is an endocrine & metabolic disorder. You should ideally be under a team of healthcare providers. A PCOS team consists of –
- Dermatologists: manage skin signs of PCOS including acne, hair, oily skin, skin tags and dark patches.
- Endocrinologist: to monitor blood sugar levels & insulin resistance.
- Gynaecologist is useful if you are planning to fall pregnant.
- Dieticians: can guide you with foods for acne management and weight loss.
Exercise physiologists: can help you lose weight & manage your BMI. Do not underestimate the value of exercise as this has a flow on effect on skin health.





