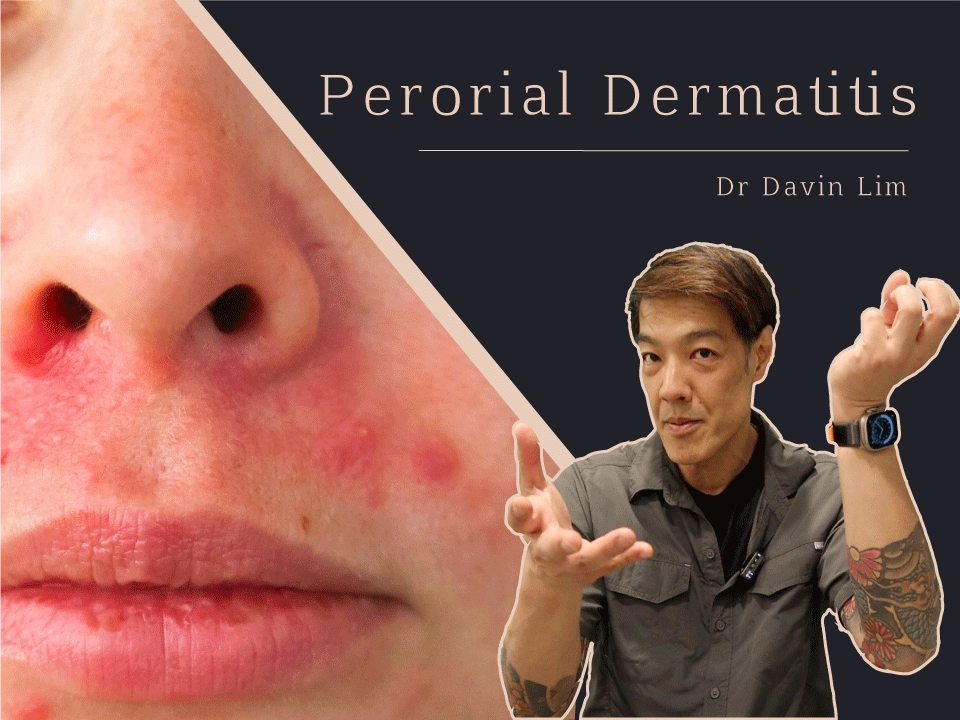
Perioral dermatitis is a common rash managed by dermatologists. This rash presents as red bumps around the mouth, nose & eyes. A dermatologist can safely & efficiently clear up this rash & prevent recurrence. Lasers can reduce redness, inflammation & repair damaged skin.
We offer a wide range of effective treatment options including:
- Perioral Dermatitis Treatment
- Skincare for perioral dermatitis
- Perioral Dermatitis Skin Repair
- Vascular Lasers
Our results speak for themselves
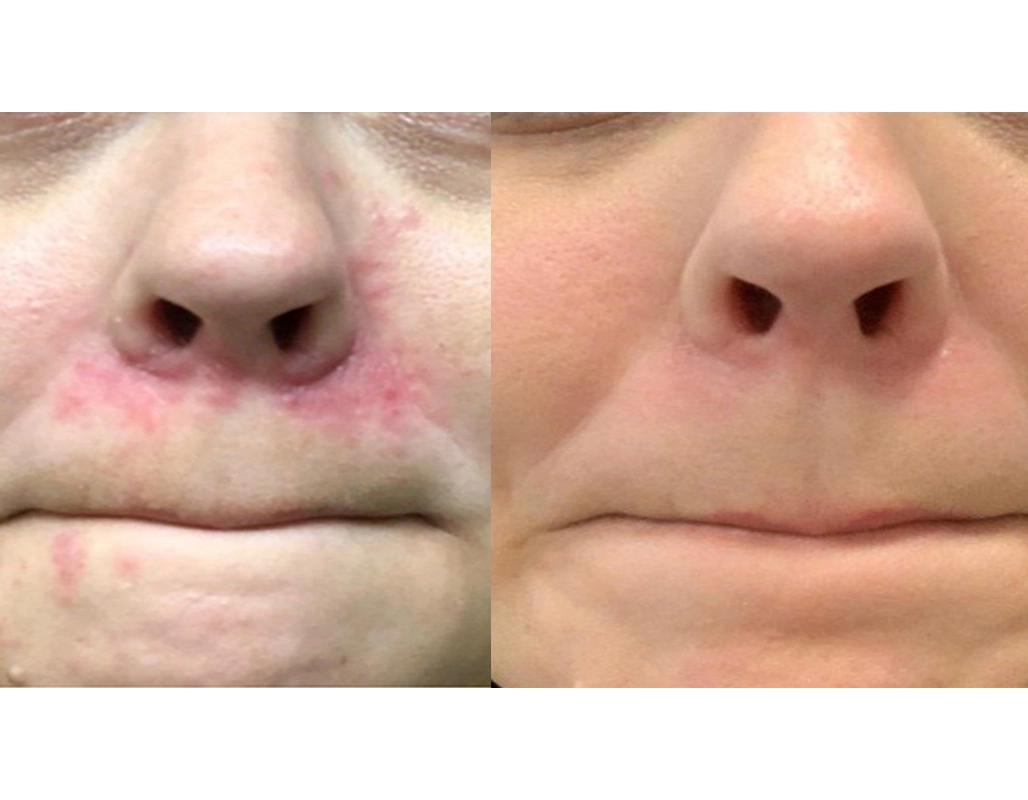
Before
After
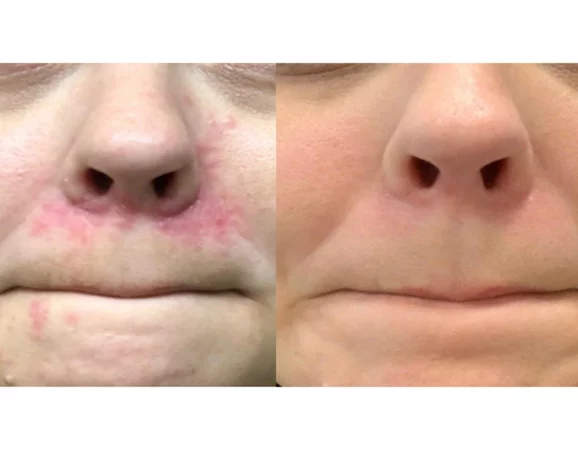
Anti-inflammatories
Ask us more about this treatmant
Preferred Consultation
Before
After
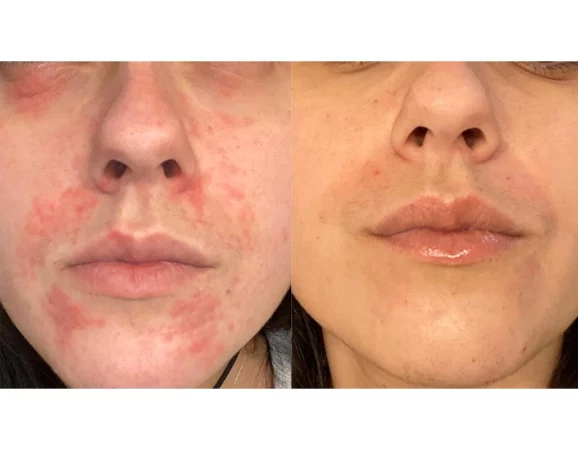
Anti-inflammatories
Ask us more about this treatmant
Preferred Consultation
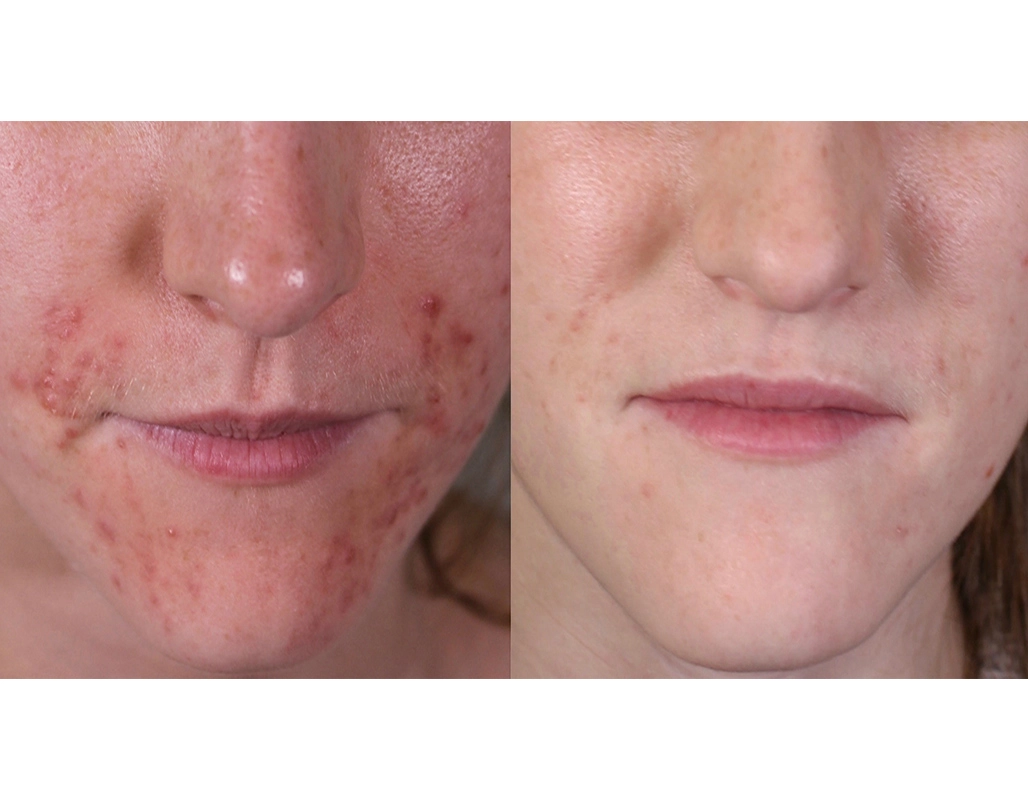
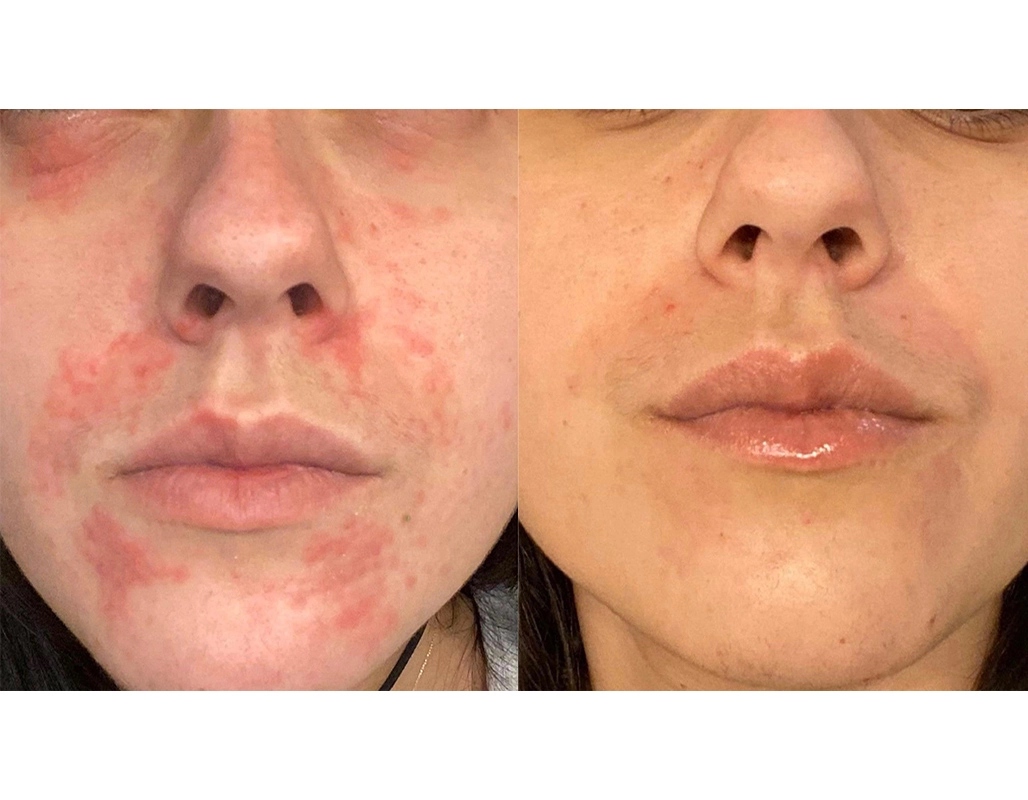
Before
After
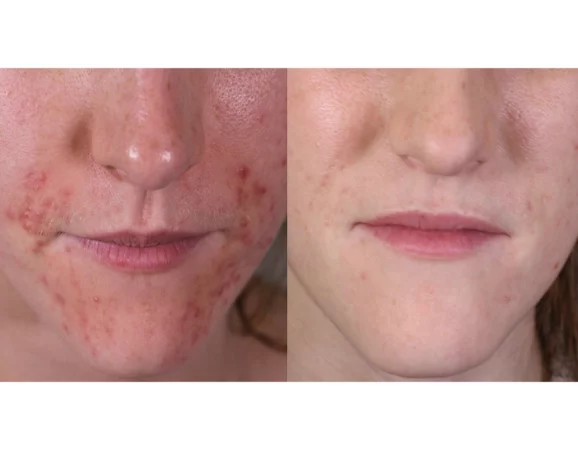
Anti-inflammatories
Ask us more about this treatmant
Preferred Consultation
Treatments for Perioral Dermatitis
Simplify your skincare routine for fast results
Effective treatment programs
A simplified skincare routine is advocated if you are prone to perioral dermatitis. Hydrating cleansers & light moisturizers with ceramides can help repair damaged skin.
Our dermatologists can guide you as the best skincare during your treatment & your recovery phase.
With specialist treatments your rash will improve within days. Our experts will tailor a simplified treatment program together with medications that quickly & safely reduce skin inflammation.
Cutis Dermatology has an urgent triage system for facial rashes, in most cases we can see you within 72 hours. Call reception & they will fit you in ASAP to see our experts.
Reduce redness fast with vascular lasers
The correct skin care will stop perioral dermatitis from recurring
Skin takes time to recover from inflammation caused by dermatitis. Cutis Dermatology has the latest in laser technology designed to repair damaged skin. Gentle vascular lasers can reduce redness & accelerate healing.
Choosing the correct cleanser, moisturiser, & skincare actives will reduce the chances of perioral dermatitis from coming back. Our expert team will advise you on the correct range of affordable anti-aging skin care for your skin type.
Finding a simple, yet effective skincare routine can prevent the recurrence of perioral dermatitis. Our specialists can guide you as to the best products for your skin.
FAQs
What is perioral dermatitis?
This common rash typically occurs around the mouth & nose. Periocular dermatitis is a variant that occurs around the eyes. It is classified as an inflammatory disorder of the skin.
How do dermatologists diagnose perioral dermatitis?
In 96% of cases the diagnosis is clinical, meaning no tests are required.
In unusual cases they may order special tests to tell the difference from granulomatous rosacea, tinea incognito, granuloma faciale, lupus miliaris & atypical rashes.
Will dermatitis go away by itself?
It may, but this can take months to years. Treatment courses of 4-6 weeks duration can clear up most cases.
How to stop the itch & burning?
Your dermatologist will base treatments on your signs & symptoms. Most cases will settle within a few days. Cool compresses can help. In severe cases your dermatologist may give you a very short course of topical anti-inflammatories.
What cleansers should I use?
A non-irritating bland cleanser is best. La Roche, Cerave & Cetaphil are good cleansers. Above all avoid BHA/AHA cleanser & toners during the treatment phase.
What moisturizer should I use if I have perioral dermatitis?
Preferably a light one. Your dermatologist will advise you accordingly. Brands include Cetaphil, La Roche Posay, Obaji, & Aspect Dr.
Do I have to stop using makeup?
Ideally yes, but only for a week or two. This can accelerate the results of treatment. Be guided by your dermatologist. Oil based makeup is not advisable, mineral makeup is better if you are prone to getting perioral dermatitis.
How long till POD gets better?
1-2 weeks. If you are on a steroid preparation, it may flare up for a week before improving. Follow your dermatologist advice, & you will be fine. It’s important to take the course of medication to ensure it doesn’t come back.
Does perioral dermatitis scar?
No, but it will leave some redness behind. This can take 4-6 months before disappearing. One to three simple vascular laser treatments can repair the skin & reduce redness.
Will perioral dermatitis flare up if I stop steroid ointments?
If you have been prescribed topical corticosteroids, you may have a transient flare up upon cessation. Don’t stress, continue to your prescribed treatment plan. Flare ups typically take 5-12 days to settle down.
Will I need to stop all skin care actives, including sunscreen?
Yes. Most dermatologists will ask you to temporarily stop sunscreen for a short period, ranging from a few days to a week or two. You’re not going to age exponentially by doing so.
What are other rashes that look like perioral dermatitis?
POD is classic, especially if there is a history of steroid use, however other rashes may resemble perioral dermatitis, including-
- Acne rosacea; usually has blackheads & or symptoms of rosacea
- Seborrheic dermatitis; usually has scalp or brow involvement
- Allergic or irritant dermatitis; may require allergy testing
Does it occur in children?
Perioral dermatitis is frequently seen in children, the most common causes include corticosteroid use, including creams & inhalers. Treatment is per adult cases apart from the antibiotic we use.
Will perioral dermatitis come back?
Most cases don’t, providing flare factors have been identified & avoided. 10-20% of patients have recurrent POD, possibly due to the wrong makeup, cleanser, moisturizers & skin care.
Our team will advise you on the best solutions for your skin type.
What happens if it comes back?
Your dermatologist will figure that out. They may-
- Extend your course of anti-inflammatory medications
- Change your skin care & products
- Change medications & add lasers
- Think of other rare diseases that look like perioral dermatitis
- Consider patch testing
- Ask you to change your toothpaste
Is it contagious?
No type of dermatitis is contagious. It can’t be transmitted to another person.
Is perioral dermatitis an infection?
Though the exact cause is unknown, candida yeast & follicular infection with fusiform bacteria have been implicated. The prescription given to you by your dermatologist does not target infectious processes but reduces skin inflammation.
Is perioral dermatitis food related?
Food is not a causative factor for perioral dermatitis. However, in some cases hot spicy food can irritate skin, worsening the rash. Acidic fruit juices are frequent irritants.
Allergies to food, metals & fluoridated toothpaste may present as perioral dermatitis like eruptions. In suspected cases your dermatologist may arrange allergy tests.
What can lasers do?
Lasers are not the primary treatment choice; they can however reduce background redness & help repair the skin due to inflammation.
Vascular lasers are the most used devices. Treatment takes a few minutes to perform, makeup can be worn the next day. Our nurses perform this procedure.
What's the best natural remedy for perioral dermatitis?
There are no scientific studies based upon natural remedies, however if you would like to give it a go you can try-
Azelaic acid twice a day for 6 weeks. It works in 20-30% of cases. This is technically organic as it is found in wheat, fungi & plants. Don’t try tea tree oil.
How to treat perioral dermatitis in pregnancy?
Safely. The best way is with azelaic acid or topical erythromycin & pulse dye laser. You can negotiate oral therapy with your obstetrician (erythromycin).
What’s the final checklist for perioral dermatitis?
Stop the following:
- Topicals
- Face creams, including moisturizers, toners, scrubs, masks
- Cosmetics including makeup
- Sunscreen
- Fluorinated toothpaste
Commence on treatments as prescribed by your dermatologist, including
- Simple cleansers
- Superlight moisturisers
- Medication for 3-6 weeks as directed
- In most cases you can apply light makeup & sunscreen at day 14-21
What is the cause of perioral dermatitis?
It’s complex. In most cases there are at least 2-3 factors in play.
Steroids & medications
- Steroid creams, lotions
- Inhaled spays
Cosmetics:
- Moisturizers & heavy creams.
- Fluorinated toothpaste.
- Oil based makeup
- Too much makeup
Other:
- Hormonal changes
- Skin barrier problems
- Problems with the immune system.
- Candida albicans, demodex, bacteria
The most common cause is prescription steroids for a primary non-specific rash like seb dermatitis or irritant contact dermatitis (not allergic). From there, patients develop a steroid dependence. POD ensures & the rest is history.