Our team of dermatologists have successfully treated thousands of psoriasis patients over the past 25 years of practice. We treat all forms of psoriasis including scalp, facial, hand & foot, as well as paediatric cases.
We offer a variety of approaches to treating psoriasis, including:
- Narrowband Phototherapy
- Vitamin A therapy
- Vitamin D therapy
- Creams for psoriasis
- Tablets For Psoriasis
- Psoriasis Diet
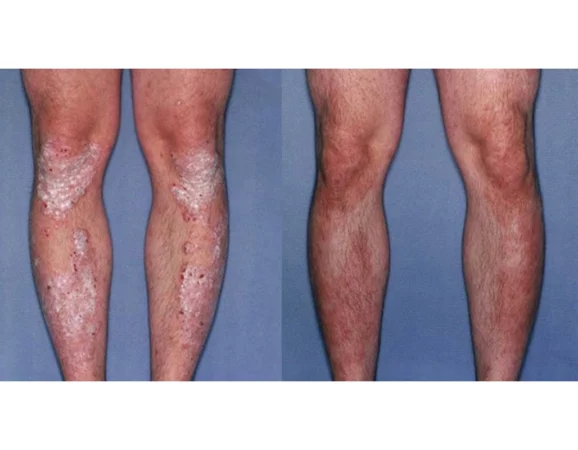
Our results speak for themselves
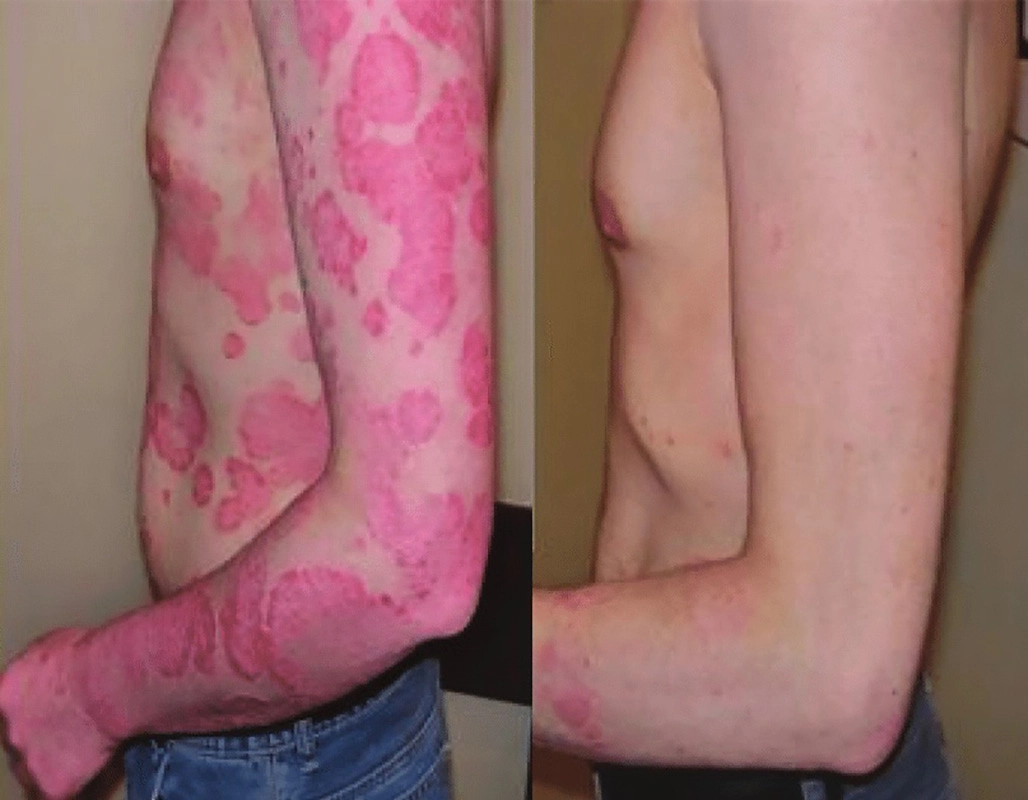
Before
After
Phototherapy psoriasis protocol
Ask us more about this treatmant
Preferred Consultation
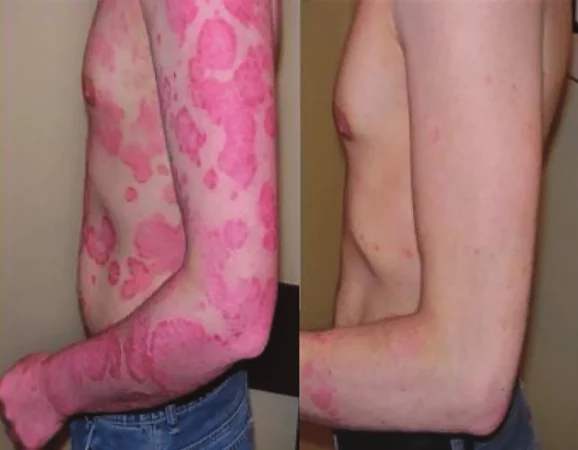
Before
After
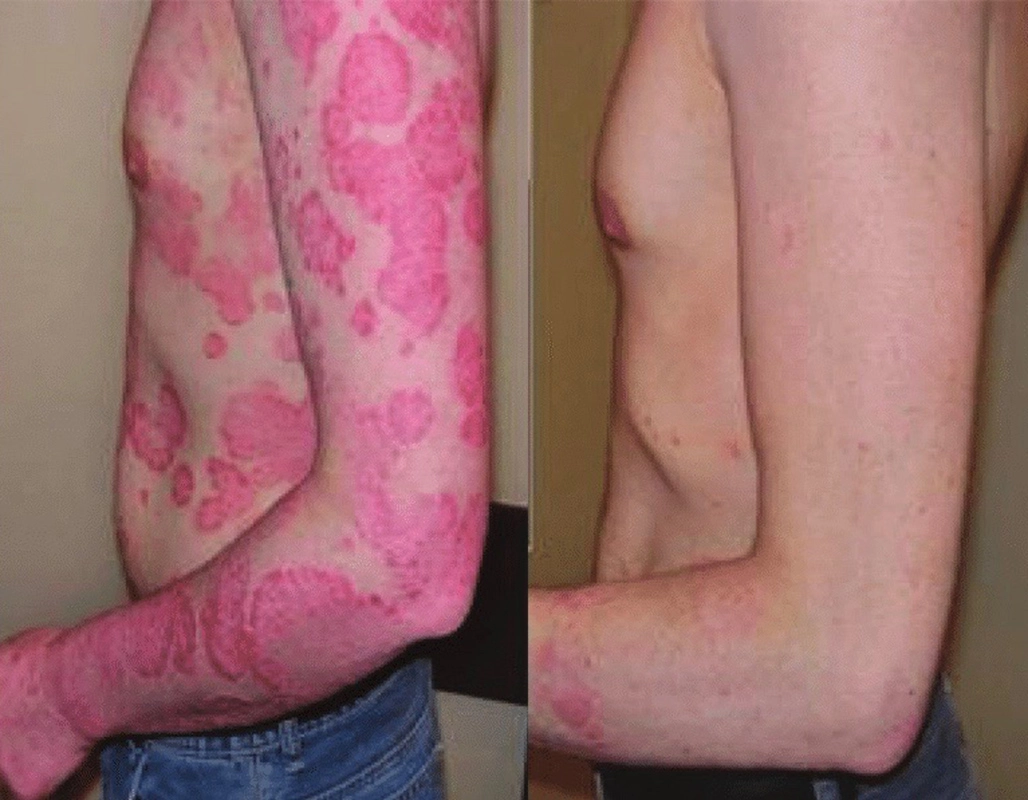
Phototherapy can treat psoriasis whilst
reducing the side effects of topical
steroids
Ask us more about this treatmant
Preferred Consultation
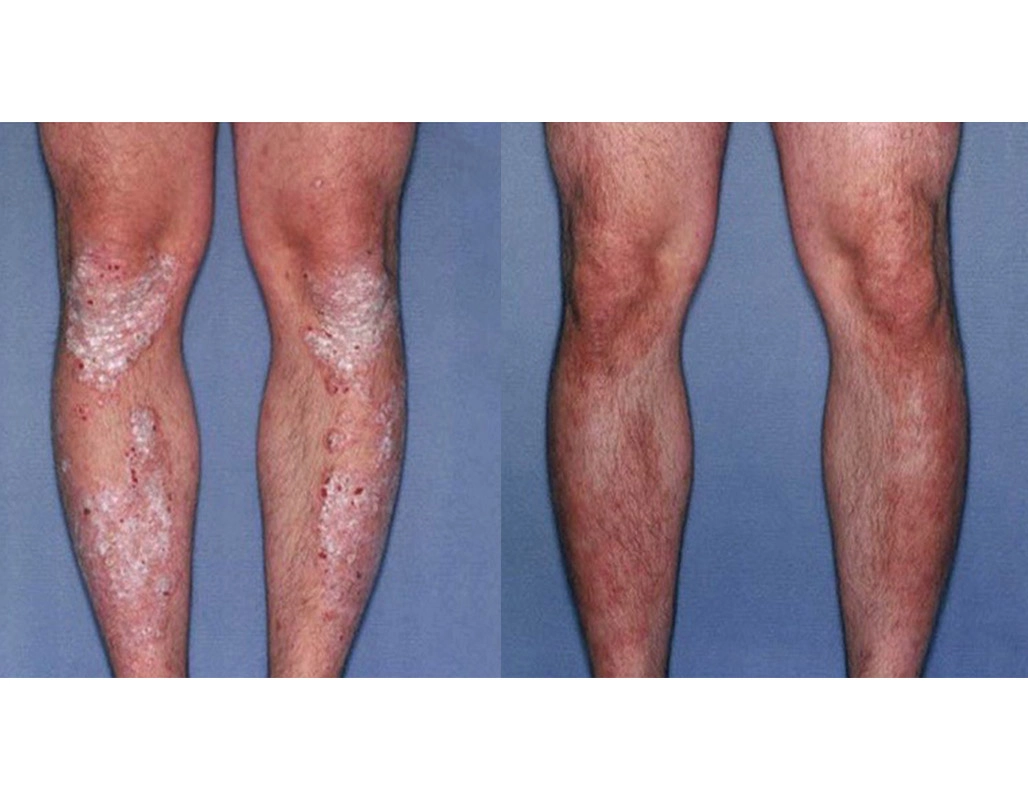
Before
After
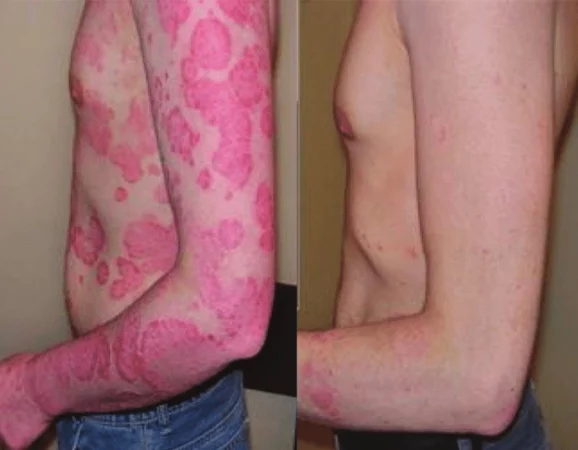
Phototherapy psoriasis protocol
Ask us more about this treatmant
Preferred Consultation
Psoriasis Treatments
Psoriasis experts
Healing with light. The power of phototherapy
Our team of dermatologists have treated thousands of psoriasis patients over the past 25 years of practice. We have a holistic approach to treating psoriasis, including the use of vitamins A & D, creams, medications, phototherapy & dietary supplementations.
Medical phototherapy efficiently delivers UV in a safe but highly effective treatment called narrowband phototherapy. This treatment reduces the need for long term corticosteroids. Treatments take less than three minutes to perform & are covered under Medicare.
Vitamin A & psoriasis
Vitamin D & psoriasis
Vitamin A can reduce the amount of scaling due to psoriasis. This treatment is frequently combined with light therapy to reduce skin inflammation & repair damaged skin cells. Dermatologists use both vitamin A creams & tablets.
Vitamin D is a natural molecule that regulates how fast your skin cells multiply. In psoriasis patients, skin cells multiply at three to five times the normal rate. Dermatologists use vitamin D creams, gels & lotions to help slow down cell turnover.
Vitamin D can be used on the skin, scalp & nails, depending on the formulation.
Our team of dermatologists have treated thousands of psoriasis patients over the past 25 years of practice. We have a holistic approach to treating psoriasis, including the use of vitamins A & D, creams, medications, phototherapy & dietary supplementations.
FAQs
What is Psoriasis?
Psoriasis is a chronic inflammatory disease, primarily affecting the skin, & occasionally affecting the nails & joints. It does not scar the skin but can sometimes cause an increase or reduction in skin pigmentation. It can present on all parts of the body.
What causes Psoriasis
The actual cause of psoriasis is a rapid turnover of skin cells. Normal skin cells shed over one month, in psoriasis, it’s just 4-5 days. Other factors include-
Genetics: as it often runs in families
Infection triggers: such as strep & staph
Stress: can make any medical condition worse
Medications: such as beta blockers, lithium & steroids. Nicotine & alcohol.
Foods: are very rare flare factors, including gluten & acidic foods
How common is it?
Psoriasis occurs in all ethnicities. It affects about 2% of the population. Most cases occur in young adults, but children & the elderly can be affected.
How do our dermatologists manage psoriasis?
Cutis Dermatology in Brisbane comprises specialist nurse practitioners, dermatologists, & a referral team of rheumatologists, cardiologists, & dieticians who can work together to address all the issues associated with psoriasis for you.
Treatments for your psoriasis include-
- Identifying & avoiding triggers– our team can help you identify and treat your triggers including allergies, irritants, stress & trauma.
- Screening for associations – our multidisciplinary specialist team will screen you for diseases associated with psoriasis, organise the required tests and organise management plans and treatment.
- Creams– in early or limited plaque psoriasis, creams may work very well. Steroids, vitamin D and A, tar and dithranol creams may be prescribed in combination to you by our specialists for this stage of psoriasis.
- Narrowband UVB phototherapy– “light treatment” is one of the best ways to treat chronic plaque psoriasis. Combined with creams or tablets, psoriasis may start to improve over a few days. This treatment can reduce the need for steroid creams. Phototherapy treatments are bulk-billed, and take no longer than 2-3 minutes to perform.
- Tablets– tablets are used in resistant or severe psoriasis, or if psoriasis is involving the joints.
- Biologic injections– this form of treatment is reserved for patients who have severe psoriasis and have failed most other treatments. At the Psoriasis Institute, dermatologists with a special interest in biologic therapies will assess and treat you if you qualify for these drugs.
How do dermatologists diagnose psoriasis?
A Dermatologist will often diagnose the condition by visually examining your skin, nails & scalp. 95% of cases do not require a skin biopsy, however in a minority we may take a sample of your skin for testing.
What are the classic skin signs of psoriasis?
Chronic plaque psoriasis which affects the knees, elbows, torso & scalp. Spots & patches are pink or red with silvery-white scales.
What are other less common skin signs of psoriasis?
- Guttate psoriasis which are small plaques of the condition scattered over the torso and limbs.
- Flexural psoriasis, affects the groin & under breast area
- Palmoplantar psoriasis which affects the hands and feet.
- Pustular psoriasis which affects the torso and limbs with tiny pus spots.
- Geographic tongue, as the name implies.
- Nail involvement only.
- Scalp involvement only.
How can psoriasis affect my nails?
Psoriasis can affect all aspects of the nails, including the nail fold, the nail plate and the matrix. Depending on which part of the nail psoriasis affects, the findings may differ.
Pitting of the nails is the most common finding- tiny pits may be seen on the nail plate, and may affect the finger and toenails.
Crumbling and thickened nails may occur on a few nails, or in severe cases all nails.
Discoloration of the nails may be the only sign of psoriasis. This may give a dirty or oily look in the nail bed. Discoloration may be seen in one or two nails or affect all nails. Many patients who have this form of nail psoriasis may have been treated for a fungal infection in the past.
What is the cause of nail psoriasis?
Nail psoriasis can affect up to 50% of psoriasis patients. The cause is thought to be genetic, made worse with trauma & stressors.
The different clinical presentations of nail psoriasis depend on which area of the nail is being affected. In some cases, removing the traumatic cause can improve the nails without the need for medication.
What treatments are available for nail psoriasis?
General nail care for psoriasis patients forms the basis of treatment. Trimming nails and protecting from trauma can improve the nail disease without the need for treatments. Nail clippings should be done to ensure that the condition is not due to fungus, which may mimic nail psoriasis.
As psoriasis affects the nail when the nail is being formed, any form of treatment may take months to be effective. The nail plate acts as a barrier, so creams to this area have limited success. Creams are best applied to the nail folds.
- Vitamin D creams and solutions (Calcipotriol) can be applied twice a day to the nail folds.
- Vitamin A creams can be used in the same manner.
- Steroid creams can be used successfully, but only under medical supervision.
- Phototherapy of the hands and feet may improve nail psoriasis, especially if the nail folds are involved.
- Tablets such as Methotrexate, retinoids and biologics usually provide the most success, but side effects need to be considered.
The treatment of nail psoriasis is individualised for each patient, the specialists at Cutis Dermatology in Brisbane will discuss options with you.
How does psoriasis look like on the hands and feet?
This form of psoriasis can be difficult to diagnose, as it may mimic conditions such as hand dermatitis, or even fungal infection.
As the name suggests, psoriasis of these areas can present as red, scaly patches, often with fissures & cracks affecting hands or feet, or in some situations, both areas. Occasionally yellow pustules may occur, and over time turn into brown- black spots.
Psoriasis in these areas may cause significant pain, itchy or maybe ‘burning’ in sensation. Over time painful cracks may develop.
Treatments follow similar algorithms as treating psoriasis elsewhere.
What are the side effects of biologic treatments for psoriasis?
Because these drugs have been developed to affect only specific parts of your immune system, side effects are usually less common. However, side effects when they do occur may be more serious. Your dermatologist must ensure that you have not been exposed to certain infections such as tuberculosis and hepatitis before starting you on this medication.
New ‘biologics’, with even more specific immune effects & hopefully fewer side effects, are being developed. Your dermatologist will guide you in the most appropriate treatment.
How does Infliximab work?
Infliximab is a “biologic” designed to block tumour necrosis factor (TNF) which in the skin leads to the formation of psoriasis plaques & inflammation. The drug binds directly to circulating TNF in the bloodstream and in psoriatic skin thereby reducing the action of TNF in the development of psoriasis.
It is used in treating psoriasis, rheumatoid arthritis, psoriatic arthritis & inflammatory bowel disease. It has a rapid onset of action so it can be beneficial for unstable severe psoriasis or psoriasis requiring rapid control.
Infliximab is usually given to patients in a specialised treatment centre in a hospital or doctor’s clinic. It is given as an intravenous infusion straight into the blood stream every eight weeks. The infusion takes about 2 hours to complete. Patients are often monitored for side effects for a short while after the infusion is given and then are allowed to go home.
In some patients treated with infliximab, methotrexate may also be given to help maintain the effectiveness of the infliximab.
Can we treat genital psoriasis?
Genital psoriasis can present as red, scaly patches on the penis & genital areas. It can affect the head & shaft of the penis, scrotum, pubic & anal area. Burning, stinging & skin irritation are common. Treatment for psoriasis may include topical medications, light therapy, and oral medications. A dermatologist can diagnose & effectively treat psoriasis.
Learn more here – This page is written in the context of diagnosis & treatment of psoriasis in males. Our specialists at Cutis Dermatology manage all forms of psoriasis.