Melanoma is the most dangerous of all the skin cancers & accounts for the majority of skin cancer deaths. Queensland has one of the highest rates of melanoma skin cancer in the world. Detected early, the cure rate is very high. Early detection saves lives.
Key Points
- Brisbane has one of the highest rates of melanoma in the world
- The first sign of a melanoma is usually a change in a freckle or mole
- Half of all melanomas present as a new spot on normal skin
- Early melanomas, called in-situ cancer has a very high cure rate
- Late-stage melanoma has a very high mortality rate
- Regular skin checks saves lives
Melanoma Skin Check at a glance
Our results speak for themselves
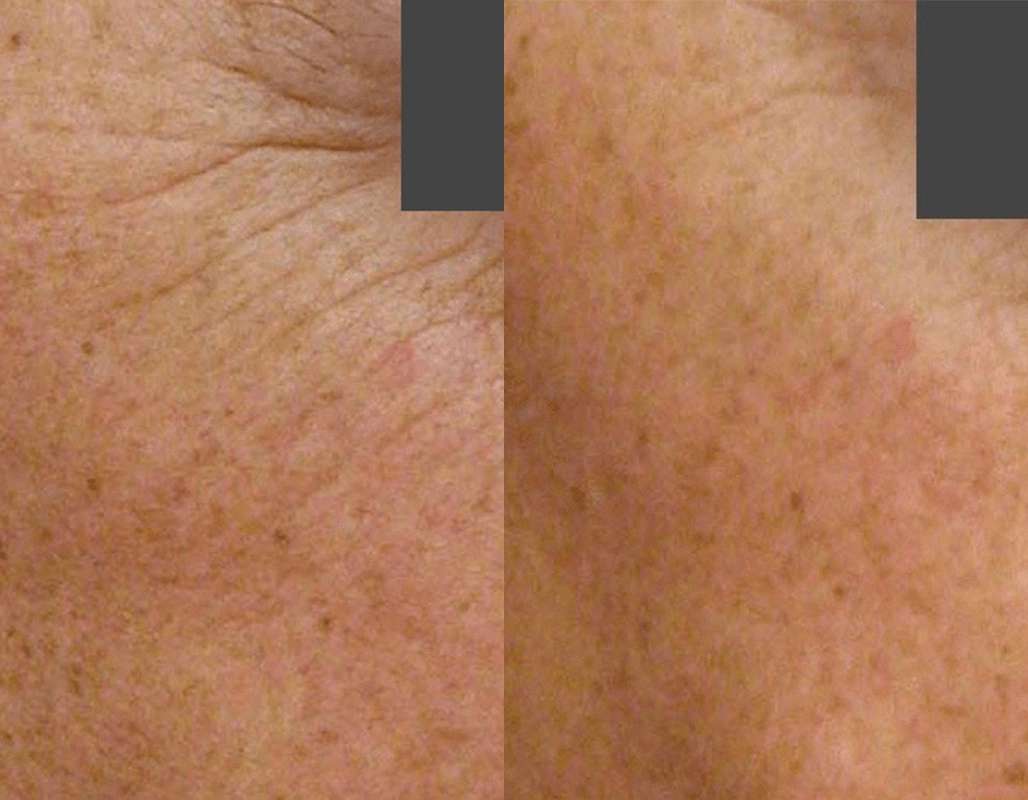
Before
After
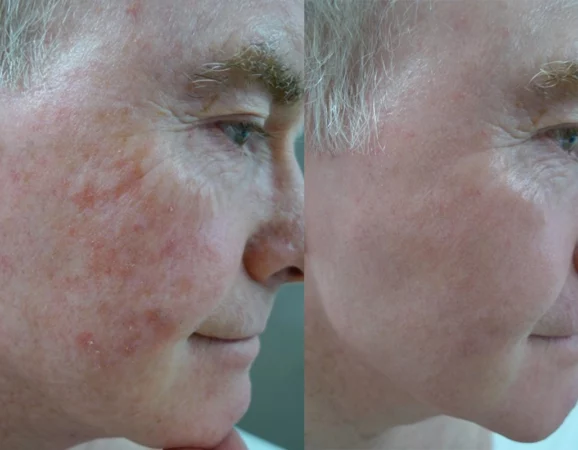
Erbium nano-micro-laser-peel. 5 days
downtime. Suitable for sun damage &
pigment in lighter skin types
Ask us more about this treatmant
Preferred Consultation
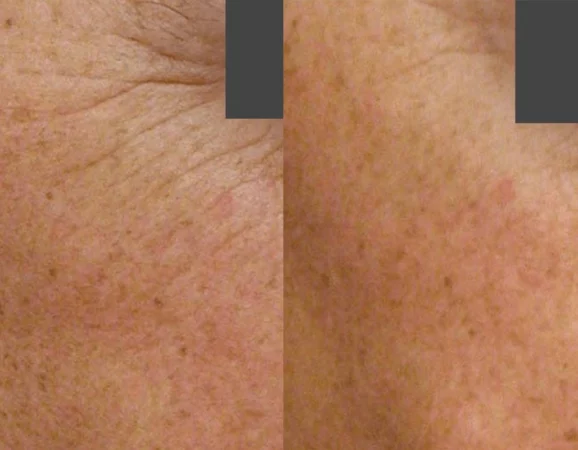
Before
After
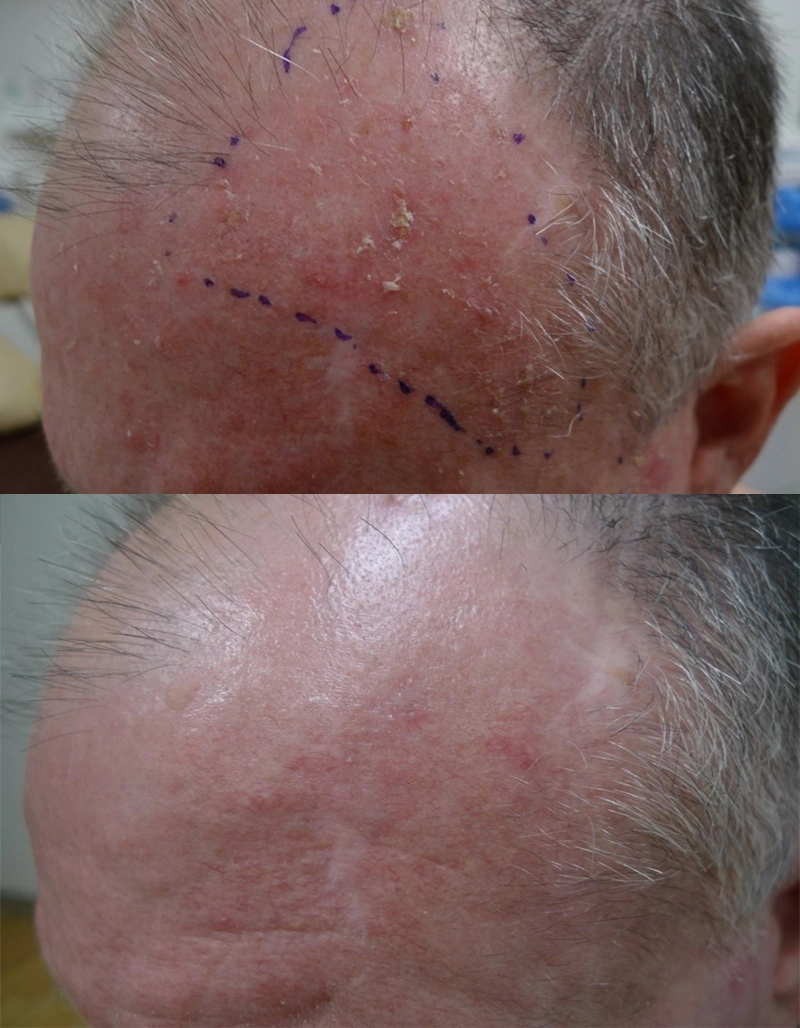
Thulium HD, 1927 overpass. 1 session
Ask us more about this treatmant
Preferred Consultation
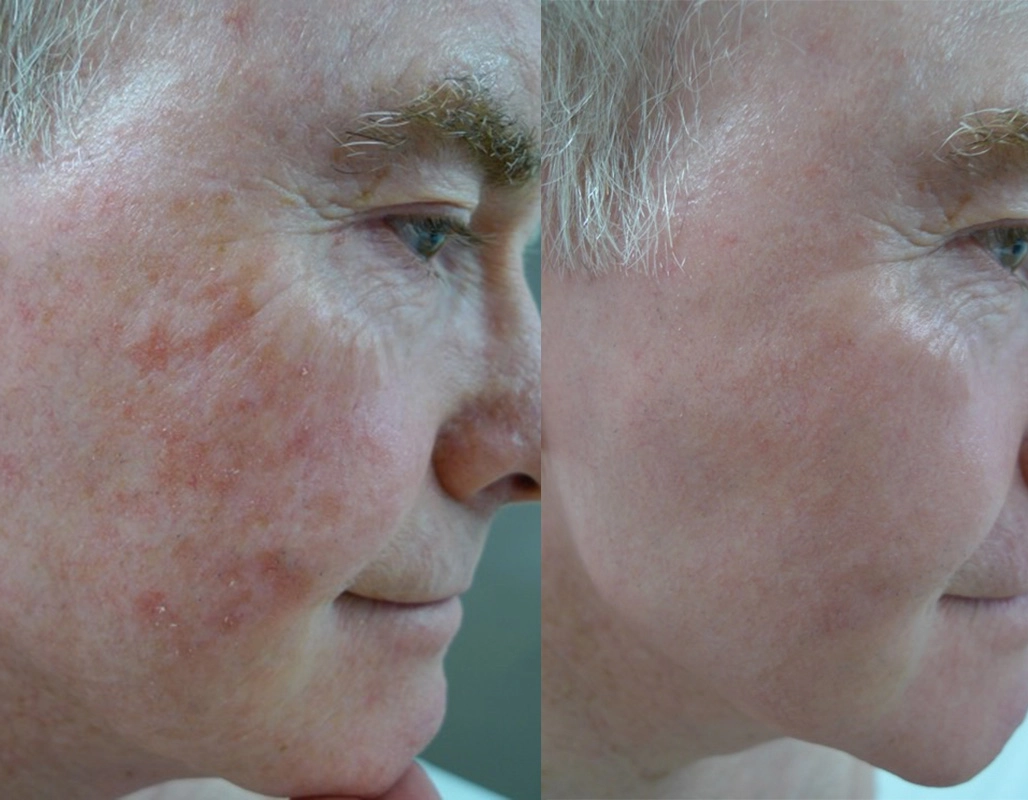
Before
After
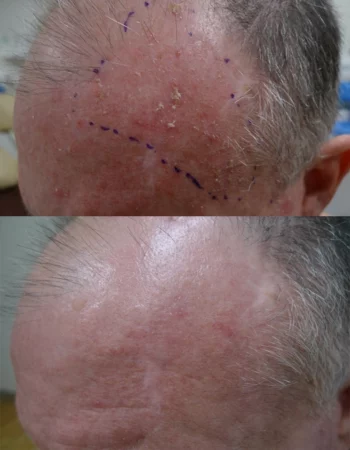
PDT
Ask us more about this treatmant
Preferred Consultation
FAQs
What are melanoma skin cancers?
Melanoma is a potentially invasive form of skin cancer. It arises from the pigment cells called melanocytes that reside in the base of the skin. In a melanoma the melanocytes become malignant & multiply excessively.
An important cause of melanoma is exposure to too much ultraviolet radiation from sunlight & or artificial sources of ultraviolet light, such as sunbeds.
How do we diagnose melanoma?
The first step is a clinical examination. If a dermatologist is suspicious, we may perform a skin biopsy & subsequent microscopic examination by a pathologist.
The diagnosis of melanoma can only be confirmed by examining the specimen.
What does a melanoma look like?
Melanomas tend to resemble a mole that is undergoing changes in shape, size, or colouration. 50% of melanomas occur in a pre-existing mole, but around half the time they arise in an area or normal skin.
Most melanomas follow the ABCDE rule (see below), however nodular, desmoplastic & amelanotic melanomas don’t follow any rules. Fortunately, these variants account for the minority of skin cancers.
Can melanomas arise in areas that don't see the sun?
Though more common in sun-exposed areas, melanomas can arise in sun-protected areas including the soles, palms, mucosal surfaces & even the nail bed. When undergoing a full skin examination, your dermatologist will examine these areas.
Need an urgent referral to see a specialist?
Our consultant dermatologists at Cutis Dermatology Brisbane have ‘hold for urgent’ spots. In most cases we can see you within 72 hours. You can access this rapid access service via your general practitioner.
If a skin cancer is suspected, we will undertake a biopsy on the day. Results can be expected within 24 to 48 hours of biopsy.
What are the chances of melanoma recurring?
If you have already had melanoma, there is a chance it may recur, hence the requirement for frequent checks. You are also at a higher risk of getting another melanoma at distant sites.
Your dermatologist will discuss this with you and will regularly monitor you for signs it has returned.
How to treat a melanoma?
All melanomas are treated by excision. The tumour is assessed under the microscope. The next step will depend on the Breslow thickness.
In most cases a further operation will be required to obtain margins. This is known as wide local excision. The extent of this surgery depends on the thickness of your melanoma.
If the melanoma is deep, we would also consider biopsy of the lymph glands. Should there be melanoma present in the lymph glands, further surgery will be required.
How is melanoma graded?
The early form of melanoma is called lentigo maligna melanoma. Treated early, this type of melanoma is almost always cured.
For more advanced melanoma the depth of invasion that tells us how the disease might behave. This depth is termed the ’Breslow thickness’. This index will determine whether you require a simple excision or furthermore complex surgery including lymph gland biopsy. The degree of spread a melanoma has undergone will be classified by stages:
Stage I: Localised to the original site only
Stage II: Localised to the skin only plus local skin spread
Stage III: Spread to the nearby lymph glands
Stage IV: Spread to the internal organs of the body
Products

O Cosmedics cleansing range
$63.00-$64.00

O Biotics 3D Hyaluronic Serum
From $97.00
Queenslanders have one of the highest melanoma rates in the world. We employ dermatoscopic examination, serial photography as well as algorithm based follow ups to pick up early signs of cancer. Early detection saves lives.
How often should I get my skin checked?
The time frame depends on your risk factors. As a guide-
- High risk patients: 3 months
- Moderate risk: 6-9 months
- Low risk: 12-18 months
Your dermatologist will guide you according to your history, previous pathology & importantly your clinical examination.
Should you get a skin check if you have ethnic skin / Asian skin type?
The chances of melanomas occurring in darker skin types are very slim. Most new spots in darker skin races are benign age warts. Melanomas in darker skin patients tend to arise in the nail beds, palms & soles. Non-melanoma skin cancers, namely pigmented basal cell cancers, are much more common than melanomas.
Bottom line, based on probability, the lesion is unlikely a melanoma, however a skin check can be helpful in relieving the anxiety.
How can mole mapping help?
If you have multiple dysplastic moles & are of higher risk for developing melanomas, your dermatologist will action Mole Mapping. This is a professional method to keep track of multiple moles.
Mole Mapping can-
- Potentially pick up melanomas earlier
- Monitor moles & other lesions
- Pick up non-melanoma skin cancer
- Reduce the requirement for multiple excisions & biopsies
What are some self-examination tips?
When performing a self-examination for skin cancer, you are looking for any changes to the size, colour of shape of your moles. You are also looking for itching, bleeding, tingling, or crusting of moles which are signs you need to book an appointment to get your moles checked by a specialist. When checking for moles, know your ABCDEs and get your moles professional checked if:
A: Asymmetry – the mole looks unusual & irregular
B: Border – the border becomes ill-defined or irregular
C: Colour – more than 2 colours appear in the mole including brown, black or light areas giving a mottled appearance. A very dark or black appearance can occur
D: Diameter – if a mole is enlarging it should be reviewed
E: Evolution – changes in size, colour, shape or symptoms
Why are nodular melanomas tricky?
Nodular melanoma doesn’t follow the ABCD rule, but it does follow the ‘E’ for evolution. These melanomas are progressive & changing, though their colour & symmetry are often banal. In the early stages the lesion may be itchy, or just feels weird.
This type of melanoma is more common in men over 50. Because nodular melanomas grow very rapidly, it can invade very quickly (within a few months). Hence the importance of early diagnosis & removal.
What is the survival rate of melanoma patients?
Survival rate is largely dependent on the depth of the melanoma – the thinner the lesion, the better the outcome. For example, a person diagnosed with a superficial in situ melanoma has over 99% five-year survival rate.
Melanoma less than 1mm thick can expect to have a 92% ten-year survival rate.
If the melanoma is greater than 4mm thick, the ten-year survival rate reduces to 50%.
What is lentigo maligna?
Lentigo maligna is a very thin melanoma confined to the upper layers of skin. It is also known as in-situ melanoma or HMF Hutchinson melanotic freckle. This type of melanoma is found on the head & neck as well as exposed areas of the body.
The rate of change into an invasive melanoma is about 5%. Detected & treated early, this form of melanoma has almost a 100% cure rate.
Who gets lentigo maligna?
This is the most common variant of melanoma in Australia. Risk factors include sun exposure, sun damage & age. Multiple NMSC & solar damage are markers for HMF lesions; however they are not precursors.
Lentigo maligna is more common in males than females. Most HMFs are seen in more elderly patients, between 60 and 80 years. Lentigo maligna is not related to the number of abnormal or dysplastic moles.
How do we treat lentigo maligna melanomas?
Excision is the preferred method. The ideal margin is between 5-10 mm, depending on site, age & other patient factors. It is not infrequent to have a sub-clinical extension of in-situ melanomas, hence the need for serial (multiple) excisions. Mohs, frozen sections, or delayed closure are all methods employed by dermatologists & plastic surgeons to increase the chances of complete excision & cure.